Article I: General Policies & Procedures
The Indiana University (IU) Master of Physician Assistant Studies (MPAS) Program Handbook and Policy Manual is designed to give you, the student, general information regarding the IU MPAS program. Students should keep this manual in a convenient location to refer to it throughout the student’s PA training. This manual provides vital information about the IU MPAS Program and the PA profession.
As a beginning PA student, you are entering into the health professional world. You will be afforded respect and honor as a PA. With this respect comes a great deal of responsibility. Most PAs look back at their experience as a PA student as one of the most challenging and rewarding times in their lives. The IU MPAS leadership is confident you will regard becoming a physician assistant as one of your life’s most significant milestones. The IU MPAS faculty and staff are dedicated to our students’ success and wish you a bright future as a healthcare provider.
STANDARD A3.01 Program policies are published, readily available, and consistently applied to all students, principal faculty, staff, and the program director regardless of their location.
The Accreditation Review Commission on Education for the Physician Assistant (ARC-PA) has granted Accreditation-Continued status to the Indiana University School of Health & Human Sciences Master of Physician Assistant Studies Program sponsored by Indiana University. Accreditation-Continued is an accreditation status granted when a currently accredited program is in compliance with the ARC-PA Standards.
Accreditation remains in effect until the program closes or withdraws from the accreditation process or until accreditation is withdrawn for failure to comply with the Standards. The approximate date for the next validation review of the program by the ARC-PA will be April 2027. The review date is contingent upon continued compliance with the Accreditation Standards and ARC-PA policy.
This handbook is in part based on the 6th edition Accreditation Standards for Physician Assistant Education published in September 2025. The Standards will be referenced throughout the manual as they inform and guide the curriculum, policies and procedures adopted by the Indiana University
MPAS Program.
According to the ARC-PA, these Standards were initially adopted in 1971 and were revised in 1978, 1985, 1990, 1997, 2000, 2005, 2010, 2011, 2019, 2025. ARC-PA commissioners include individuals nominated from the collaborating organizations of the ARC-PA. which include:
- American Academy of Family Physicians
- American Academy of Pediatrics
- American Academy of Physician Assistants
- American College of Physicians
- American College of Surgeons
- American Medical Association
- Physician Assistant Education Association
These Standards constitute the requirements to which an accredited program is held accountable and provide the basis on which the ARC-PA will confer or deny program accreditation.
The collaborating organizations cooperate with the ARC-PA to establish, maintain and promote appropriate standards of quality for entry level education of PAs and to provide recognition for educational programs that meet the requirements outlined in these Standards. These Standards are used for the development, evaluation and self-analysis of PA programs.
“Physician assistants are academically and clinically prepared to practice medicine on collaborative medical teams. The collaborative medical team is fundamental to the PA profession and enhances the delivery of high-quality health care. Within the collaborative medical team, PAs are medical professionals who diagnose illness, develop and manage treatment plans, prescribe medications, and often serve as a patient’s principal healthcare provider.
The role of the Physician Assistant demands intelligence, sound judgment, intellectual honesty, appropriate interpersonal skills, and the capability to react to emergencies in a calm and reasoned manner. Essential attributes of the graduate PA include an attitude of respect for self and others, adherence to the concepts of privilege and confidentiality in communicating with patients, and a commitment to the patient’s welfare.
The Standards recognize the continuing evolution of the PA profession and practice and endorse experiential competency-based education as a fundamental tenet of PA education. The Standards reflect a determination that a commonality in the core professional curriculum of programs remains desirable and necessary to offer curricula of sufficient depth and breadth to prepare all PA graduates for practice. The Standards allow programs to remain creative and innovative in program design and the methods of curriculum delivery and evaluation that are used to enable students to achieve program goals and student competencies. Mastery of program defined competencies is key to preparing students for entry into clinical practice.
The PA profession has evolved over time to one requiring a high level of academic rigor. Institutions that sponsor PA programs are expected to incorporate this higher level of academic rigor into their programs and award an appropriate master’s degree. The ARC-PA acknowledges on-going changes in the delivery of health care and in the education of health professionals. The needs of patients and society must be considered by the ARC-PA, the sponsoring institutions, and the programs. Educations must be provided in a manner that promotes interprofessional education and practice.
An environment that fosters and promotes diversity is considered essential to preparing PAs to provide service to others that is not exclusionary of any group, race, or culture. The various perspectives and resources offered by a diverse faculty, staff, and student body increase the overall impact the PA profession can have on patients and the global community.”
~Accreditation Standards for Physician Assistant Education, 5th Edition
STANDARD B1.01 The curriculum a) is consistent with the mission and goals of the program
a) Indiana University Mission Statement
Our mission is to provide broad access to undergraduate and graduate education for students throughout Indiana, the United States, and the world, as well as outstanding academic and cultural programs and student services.
We seek to create dynamic partnerships with our communities in economic, social, and cultural development to contribute to economic prosperity in Indiana and beyond. We offer leadership in creative solutions for 21st-century problems, and we strive to achieve full diversity and maintain friendly, collegial, and humane environments, with a strong commitment to academic freedom.
To achieve our vision as one of the great research universities of the 21st century, we will:
- Provide an excellent, relevant, and responsive education across a wide range of disciplines in baccalaureate, graduate, and professional education, to students from all backgrounds
- Pursue transformative, innovative, world-class research, scholarship, and creative activity
- Engage in the economic, social, civic, and cultural development of Indiana, the nation, and the world by building on the base of excellence in research and education.
b) Indiana University – IU Indianapolis Mission Statement
IU Indianapolis is the state’s urban research and academic health sciences campus whose mission is to advance the state of Indiana and the intellectual growth of its residents to the highest levels nationally and internationally through research and creative activity, teaching and learning, and civic engagement. By offering a distinctive range of bachelor’s, master’s, professional, and Ph.D. degrees, IU Indianapolis promotes the educational, cultural, and economic development of central Indiana and beyond through innovative collaborations, external partnerships, and a strong commitment to diversity.
c) Indiana University School of Health & Human Sciences Mission Statement
The School of Health & Human Sciences advances healthcare, kinesiology, sport, and event tourism through education, research, and community engagement. Leveraging its urban location, university reputation, deep community partnerships, and highly regarded faculty, the school prepares students to influence the future of these professions through a variety of degree offerings and scholarly activities.
d) Indiana University Master of Physician Assistant Program Mission Statement
Mission: The mission of the Indiana University Master of Physician Assistant Studies program is to successfully educate clinically competent, collaborative physician assistants to provide patient centered care.
e) Indiana University Master of Physician Assistant Program Values
- Professionalism
- Leadership
- Collaboration
- Advocacy
- Excellence
STANDARD B1.01 The curriculum: a) is consistent with the mission and goals of the program
a) Promote student success and program completion.
b) Equip graduates with the knowledge and skills necessary for entry-level physician assistant practice.
c) Prepare graduates to understand and address implicit bias and provide clinical opportunities to work with diverse, underserved populations in Indiana.
d) Prepare graduates for evidence-based decision making and critical thinking.
e) Promote a culture of professionalism, leadership, and advocacy within the PA profession.
STANDARD B1.01 The curriculum: b) is consistent with program competencies
The IU PA Program has adapted competencies from those published by the following medical education organizations: AAPA, ARC-PA, NCCPA, PAEA, and AAMC. These are located in Appendix U.
Article I: Section B
STANDARD A1.03 The sponsoring institution provides resources in support of the program director and principal faculty, as applicable to their program role, for: b) sufficient release time and financial resources for professional development specific to their PA program faculty role c) sufficient release time and financial resources for continuing medical education (CME)
STANDARD A2.01 All program faculty, including didactic and clinical instructional faculty: a) meet program-defined academic and experiential qualifications to teach in their assigned instructional areas, b) are evaluated for effectiveness in their assigned instructional areas
STANDARD A1.07 The sponsoring institution provides the program with the human resources necessary to operate the educational program, comply with the Standards, and fulfill obligations to matriculating and enrolled students, including sufficient: a) program faculty, b) administrative staff
The IU MPAS faculty and staff are dedicated professionals who focus on preparing the student to become a Physician Assistant. Both principal and instructional faculty members teach courses based on their academic preparation and professional experience. IU takes great care in selecting qualified faculty and investing in their continued education and professional growth. Thus, faculty members attend and present at local and national workshops and conferences throughout the year. Thus, when you need to meet with a faculty member about issues related to your education it is recommended you make an appointment.
If you cannot reach your instructor or when there is a true emergency, you may contact your Faculty Advisor, the Program Director, the Administrative Coordinator, Didactic Education Director, Clinical Education Director or another instructor.
1. PROGRAM DIRECTOR
The Program Director is responsible for the oversight of the program and participates in financial planning, development and continuous review and analysis of program operations. Any issues which cannot be resolved to the student’s satisfaction with a course director or faculty advisor should be brought to the Program Director’s attention. The Program Director will meet regularly with the class representatives to discuss any concerns.
2. MEDICAL DIRECTOR
The Medical Director is a physician responsible for ensuring that classroom instruction and clinical experiences are at an appropriate level of instruction for our PA students.
3. DIDACTIC EDUCATION DIRECTOR
The Didactic Education Director is responsible for overseeing curriculum administration including didactic outcomes, methods of assessment, summative evaluations, monitoring student progress, and providing support to principal and instructional faculty as needed.
4. CLINICAL EDUCATION DIRECTOR
The Clinical Education Director is responsible for overseeing the clinical phase of the program including identification and coordination of all clinical sites and preceptors. The Clinical Education Director is also responsible for overseeing clinical course outcomes.
5. PRINCIPAL FACULTY
The principal faculty of the IU MPAS program come from diverse interprofessional clinical and educational backgrounds and are well-suited to helping PA students gain the knowledge and skills needed to become competent clinicians. Students will be assigned a faculty member as an advisor who will serve as the primary point of contact while in the program.
6. INSTRUCTIONAL FACULTY
The instructional faculty (adjunct didactic faculty and clinical preceptors) of the IU MPAS program come from diverse interprofessional clinical and education backgrounds and are well-suited to complement the principal faculty to help students become competent clinicians.
ADJUNCT FACULTY: The IU MPAS program is fortunate to have access to a large pool of adjunct faculty to assist in teaching responsibilities based on their clinical expertise. The program has many physicians, physician assistants, nurses and other healthcare providers who will provide expert lectures and clinical experiences during the program.
CLINICAL PRECEPTORS: Each student will be assigned to a Clinical Preceptor at each clinical site while on rotation during the clinical phase of the program. The preceptor will establish a student’s schedule and guide the student through the daily routine of each rotation.
7. ADMINISTRATIVE COORDINATOR
The Administrative Coordinator is essential in the daily operation of the IU MPAS Program. This person is usually able to assist students with any general questions or inquiries regarding paperwork. The IU MPAS Administrative Coordinator may also assist students in making an appointment with a faculty member if the student is unable to contact the faculty person directly.
8. CLINICAL EDUCATION PROGRAM ASSISTANT
The Clinical Education Program Assistant is responsible for assisting with matters related to program clinical rotations. Students should contact the Clinical Education Program Assistant with questions regarding rotation contact information or if a student will be absent from a clinical site for any reason.
9. COURSE DIRECTOR
The course director is the faculty member who is responsible for the day–to-day operations of this course including continuous review of student progress, final grade posting, managing final grade disputes, and supervision of the remediation process. Should a student have questions about lecture content they should contact the instructor who provided the specific lecture of concern.
Article I: Section C
SECTION C: ADVISEMENT
Upon matriculation, students are assigned to a faculty member who will act as an advisor. The faculty advisor will meet with each student during the didactic semesters, as scheduled during clinical semesters, and on an as needed basis. Each student must take responsibility for their own learning and will be asked to self-evaluate individual progress by completing the Pre-Advising survey prior to meeting with their faculty advisor. Evaluations and surveys will be placed in the student academic files.
Any student with an academic concern should address the issue first with the course instructor or course director. Should the student require further assistance, the student should consult with their faculty advisor. The advisor may involve the Didactic Education Director, Program Director or other University administrative personnel as the situation warrants.
A faculty advisor will assist in identifying areas of strengths and weaknesses to help a student focus on the student’s studies. When an academic problem arises, the advisor will discuss the issue with the student to identify options and devise a plan of action.
The Program Director, Medical Director, or Principal Faculty must not participate as healthcare providers for students in the program, except for in emergency situations. Medical problems should be directed to Student Health Services or another health care provider. (Standard A3.06)
Principal faculty, the Program Director, or the Medical Director must not act as a mental health counselor for students as this constitutes participating in the healthcare of a student. The program works to have regularly scheduled advising sessions in which ensures timely access and/or referral of students to services addressing personal issues that may impact their progress in the PA program. Students who have a non-academic problem that requires formal counseling may ask an advisor to help find and access mental health services available at IU Indianapolis or the surrounding community. (Standard A3.06, Standard A3.07)
Faculty advisor schedules are varied due to clinical and academic obligations. If a student has a non-emergent need, it is best to make an appointment with the advisor via email. If a student’s need is emergent and the student’s faculty advisor is not available, the student is encouraged to contact the Program Director or another faculty member for assistance. Communication with IU MPAS principal faculty via text message is strongly discouraged.
Students must…
a) Exhibit the ability to meet the challenges of any medical situation which requires a readiness for immediate and appropriate response without interference of personal or medical problems. This requires training and/or certification for emergencies (i.e., CPR, ACLS, infection control).
b) Attend and be able to travel to and from classes and clinical assignments on time and possess the organizational skills and stamina for performing required tasks and assignments within allotted time frames. This involves frequent oral, written, and practical examinations or demonstrations. Students must have the ability to perform problem-solving tasks in a timely manner.
c) Adhere to policies of the university, the IU MPAS Program and clinical sites. This includes matters ranging from professional dress and behavior, adherence to substance use policy, and attending to the program’s academic schedule, which may differ from the University’s academic calendar and be subject to change at any time.
d) Demonstrate knowledge of and commitment to the code of ethics of the PA profession and behavior that reflects a sense of right and wrong in the healthcare environment.
e) Take initiative to direct their own learning. Students need to work cooperatively and collaboratively with other students on assigned projects and participate willingly in a supervisory process involving evaluation of abilities and reasoning skills.
Students will be required to:
a) Participate in patient assessment and evaluation.
b) Participate in invasive and non-invasive procedures.
c) Participate in emergency care.
d) Work lengthy and irregular hours attending to patients.
e) Perform physical examinations on both male and female peers along with being examined by both male and female peers during laboratory instruction.
f) Attend and participate in didactic and clinical education and training, on and off campus.
g) Analyze their performance via audio-visual recording.
STANDARD B4.01 The program conducts frequent, objective, and documented evaluations of student performance to ensure students meet the program’s learning outcomes for both didactic and supervised clinical practice experience components. The evaluations: b) allow the program to identify and address any student deficiencies in a timely manner.
Physician assistant students must recognize themselves as future clinicians providing a service to the patient. PA students must be aware that even as a student they are viewed by both patients and medical providers as part of the larger medical community. It is critical, therefore, that professionalism development be assessed just as academic and clinical skills are measured during a student’s academic and professional tenure.
Professional behavior will be monitored on a regular basis by the Student Progress Committee (SPC), through review of the Student Self-Assessment, Professionalism Development and Assessment Tool (PDAT), clinical evaluations, Incident Reports, and professionalism competencies as outlined below:
1. Student Self-Assessment: Students are required to complete the Professionalism Self-Assessment at least once during the didactic year and once during the clinical year.
2. Professionalism Development and Assessment Tool (PDAT): Professionalism behavior and development will be considered in each MPAS course using the PDAT rubric. Course directors will confer with relevant instructional faculty as needed to evaluate and provide feedback to each student utilizing the PDAT rubric. Upon matriculation, it is expected that the student display professional behavior in accordance with a Level 2 Competency.
3. Clinical Evaluations: Clinical preceptors will complete an evaluation of each clinical student.
4. Incident Reports: IU MPAS principal faculty will monitor professionalism throughout the curriculum, including documenting minor professionalism infractions through Incident report forms.
At the end of each semester, the SPC will review all the above for any unacceptable evaluations and recommend an appropriate course of action.
During the course of a semester, a significant lapse in professionalism may trigger prompt evaluation and intervention, as determined necessary by the SPC.
Violations of conduct standards are subject to disciplinary action administered by the University, SHHS, and by the IU MPAS Program. The Professionalism Review and Academic Review processes are outlined in the respective sections.
a) Statement of Values
The American Academy of Physician Assistants (AAPA) has identified four primary bioethical principles:
1) Autonomy
2) Beneficence
3) Non-maleficence and
4) Justice
These four principles form the foundation of the Statement of Values of the Physician Assistant Profession. The Statement of Values provides a guideline for ethical conduct by physician assistants. A complete discussion of the ethical conduct required of physician assistants may be found at the AAPA website, www.aapa.org.
In addition to the AAPA’s guidelines, The National Commission on Certification of Physician Assistants (NCCPA) has adopted a code of conduct for certified and certifying physician assistants. NCCPA’s code of conduct “outlines principles that all certified or certifying physician assistants are expected to uphold.” The NCCPA code of conduct may be found at https://www.nccpa.net/resources/code-of-conduct/?mID=11245T.
In addition to knowing and complying with the principles and standards promulgated by the AAPA, the NCCPA and the ARC-PA, physician assistant students are required to know and comply with the policies, procedures and rules of the IU MPAS Program, the School of Health and Human Sciences (SHHS), Indiana University/IU Indianapolis and each clinical site to which the student may be assigned.
Students are required to be familiar with the IU Code of Student Conduct found at: https://studentaffairs.indianapolis.iu.edu/student-conduct/index.html
Students are also expected to sign and submit the SHHS Honor Code (linked at the very beginning on page 3).
Article I: Section D
A career in health care requires integrity. It is expected that all students act in recognition of this requirement. Medical education is stressful, and sometimes good people are tempted to make poor decisions. If a student experiences this difficulty, the student must contact the course director/instructor or faculty advisor for guidance. This section contains information regarding expectations for academic integrity as outlined by the IU Master of Physician Assistant Studies program, School of Health & Human Sciences (SHHS) and Indiana University.
STANDARD B2.19 The curriculum must include instruction in: a) intellectual honesty, b) academic integrity, and c) professional conduct.
In order to ensure that Indiana University’s Master of Physician Assistant Studies Program graduates become competent and ethical practitioners, the program in conjunction with the SHHS Dean's Office developed the following information regarding academic honesty and integrity. This information will be reviewed with all students entering the program during orientation. It is the responsibility of the student to visit these policies regularly to maintain a current understanding.
In both academic and clinical settings, honesty and integrity are essential. As part of the SHHS’s preparation of future healthcare practitioners and as part of the mission of Indiana University, the IU MPAS program is committed to upholding the highest standards at every level. Much of what is presented and discussed in class is about ideas. Faculty use the term “intellectual property” when discussing ownership of ideas. Whenever scholars or clinicians use ideas from others or use their property, they must acknowledge ownership by citing the source of the information being used. Honesty and integrity are basic values of the IU MPAS program, the PA profession and Indiana University.
Violations of the policy on Academic Honesty and Integrityin any of its forms will not be tolerated. |
a) Definitions of Academic Dishonesty
1) Cheating
Dishonesty of any kind with respect to examinations (oral, written, electronic or practical), course assignments, alteration of records or illegal possession and/or dissemination of examination questions shall be considered cheating. This also includes providing assignment questions and answers to future cohorts. It is the responsibility of the student not only to abstain from cheating but to guard against making it possible for others to cheat.
2) Plagiarism
Honesty requires that any ideas or materials taken from another source for either written or oral use must be fully acknowledged. Offering the work of someone else as one’s own is plagiarism. The language or ideas thus taken from another may range from isolated formulas, sentences or paragraphs to entire articles copied from books, periodicals, speeches or the writings of other students. The offering of materials collected by others in the form of projects or collections without acknowledgement also is considered plagiarism. Any student who fails to give credit for ideas or materials that are taken from another source is guilty of plagiarism.
3) Complicity
The definition of complicity is assisting or contributing to academic dishonesty.
b) Penalties
Cheating and plagiarism will not be tolerated and may be grounds for receiving a zero on the assessment, course failure and/or subsequent dismissal from the IU MPAS Program.
c) Procedures
Incidents directly observed by faculty or staff, or incidents observed and documented by students are deemed actionable. The reporting student name will be kept confidential. No anonymous communication will be considered. Faculty will use the following protocol when presented with evidence of cheating, plagiarism or any other form of academic dishonesty by a student:
1) The instructor responsible for the instructional content will meet with the accused student along with the student’s faculty advisor. In the instance where the student’s faculty advisor is also the instructor, the Student Progress Committee Chair will act as the student’s advisor; if this is also the same person, the student may select a principal faculty representative to serve in the capacity as their advisor.
2) The accused student will be shown the evidence and asked for an explanation.
a. In cases of plagiarism, the student is required to bring in previous papers to check for similar instances of copying. Student must keep all returned papers while enrolled in the IU MPAS Program with professor’s feedback and be able to produce them at any time throughout the program. The student should also keep all preparatory notes, outlines, and drafts to prove, if necessary, that the paper is your own work.
3) Any concerns about plagiarism, cheating and/or academic dishonesty will be discussed at faculty meetings. The instructor will recommend sanctions to the faculty and the faculty, by consensus, will determine the sanction. The instructor will notify the student of the sanction in writing. Sanctions may include but are not limited to: receiving zero on the assessment, failure of course, and/or dismissal from program.
4) Disciplinary consequences will be documented in the student’s academic file.
All forms of dishonesty, whether by act or omission, including, but not limited to, cheating, plagiarism, and knowingly furnishing false information to the University, are prohibited.
Work submitted in courses must be the product of the efforts of the student presenting it, and contributions of others to the finished work must be appropriately acknowledged. The presentation of another’s works as one’s own is a serious violation of the academic process, and it is penalized accordingly.
In addition, the IU MPAS student must know and comply with the following guidelines included as part of the Policy on Academic Honesty and Integrity of the MPAS Program. Students are:
1) Expected to complete all course work individually unless otherwise specified by the instructor.
2) Not permitted to use notes or other materials during examinations unless expressly authorized in advance to do so by the instructor.
3) Not permitted to discuss material from an examination after the examination is administered with individuals other than the faculty responsible for the exam.
4) Required to do their own work and may never, under any circumstances, submit any-thing created by others (including papers purchased from commercial enterprises) as their own work.
5) Required to sit for examinations that are submitted to fulfill their own academic obligations. That is, students may not have another student or person take an examination for them.
6) Not to submit work more than once for credit, honors or to fulfill the requirements of an academic exercise.
7) Not permitted to review prior related examination questions or answers and/or graded assignments completed by another person.
8) Not allowed to copy or use another student’s work.
9) Required to give proper attribution when using the words or ideas of another person, whether in a written or oral academic exercise. This includes, among other things, proper citation of quoted and paraphrased material.
10) Not to falsify information to MPAS Program faculty and staff, supervisors, patients, and clinical preceptors.
11) Not to falsify any information including, but not limited to, duty logs, patient encounter logs, laboratory data, and patient information.
12) Prohibited from falsifying any document.
13) Prohibited from forging another’s name or signature.
14) Prohibited from misrepresenting oneself as a physician assistant, nurse practitioner, medical resident, and the like.
a) Acknowledge any ideas, facts, or language taken from a source. Use citations appropriately and include a reference list consistent with the discipline’s citation standards.
b) Quote—any language taken from an original source, even key words or short phrases, must be within quotation marks and quoted accurately. Reorganizing a sentence, substituting a synonym or altering a word or two does not make it your own work!
c) Paraphrase—this means summarizing the source in your own words. Remember: paraphrased ideas must still be acknowledged. To paraphrase well, you must read carefully enough to digest ideas and make them your own.
Breaches of academic integrity are regarded as serious offenses.Any breach of academic integrity may serve as grounds fordismissal from the IU MPAS Program, even on a first offense. |
Article I: Section E
IU MPAS students are expected and required to conduct themselves in a manner that complies with the following principles and standards:
Physician assistant students are expected to treat all patients and families, faculty, staff, clinical preceptors, health care workers, and fellow students with dignity and respect. Students must:
a) Recognize and embrace their role as a member of a team and interact with others on the team in a cooperative and considerate manner.
b) Maintain and exhibit respect for the privacy and confidentiality of fellow students. Physician assistant students will train closely with other students, including in physical examinations of fellow students and participation in discussion groups that may reveal personal information.
c) Offer criticism or suggestions in a thoughtful and reasoned manner which fosters respect and trust.
d) Maintain respect for team members and instructors and refrain from responding angrily.
e) Respect the authority of the instructor in the classroom and in student/instructor meetings.
f) Maintain classroom decorum defined as refraining from disruptive talking and late arrivals. Students may be asked to leave the classroom when disruption occurs.
g) Not disrupt or obstruct teaching and learning (including arriving late to class or side-talking while the instructor is trying to teach).
Physician assistant students may be required to be flexible due to changes in the academic schedule. Lectures or clinical sessions may, at times, need to be rescheduled with short notice. In addition, clinical sites create student schedules for each rotation and such schedules may require physician assistant students to work weekends, nights and holidays. It is imperative students remain available during program hours, which are 8am–5pm Monday through Friday. The program does not always follow the IU Indianapolis or university calendar.
Physician assistant students have a unique role in health care delivery. Students are accountable to:
a) Perform only those procedures authorized by the IU MPAS Program, clinical site, clinical supervisor, and/or clinical preceptor.
b) Always work under the supervision of a preceptor, never assuming primary responsibility for a patient’s care. Students shall not treat or discharge a patient without prior consultation with and approval of a clinical preceptor or clinical supervisor.
c) Attend and actively participate in all class activities, which includes maintaining visual presence during online learning when feasible.
d) Engage in independent learning with all assigned asynchronous lectures and class activities to the best of their ability.
e) Complete in a timely and effective manner all assignments to the best of their ability.
f) Identify and report unprofessional, unethical and/or illegal behavior by health care professionals, students, faculty, and/or staff of the IU MPAS Program. If a physician assistant student has a reasonable belief that such conduct has occurred, the student shall report the behavior to the Program Director, preceptor, supervisor, Clinical Education Director or Didactic Education Director as may be appropriate under the circumstances.
g) Accept and provide constructive feedback.
h) Exercise sound judgment.
Shadowing is not organized, required, or endorsed by the IU MPAS Program and is not considered part of a clinical rotation. Students who choose to participate in shadowing do so voluntarily and independently; therefore, they are not covered under the program’s liability insurance during these activities. While shadowing, students must not perform any duties or engage in any activities that constitute practicing as a PA student. Additionally, students must not wear their IU MPAS student badge, white coat, or any other identifiers linking them to the program, nor may they represent themselves in any capacity as an IU MPAS student, as the experience is not sanctioned by the program.
Physician assistant students must demonstrate concern for the patient. Concern for the patient is manifested in many ways including, but not limited to, the following:
a) Treating patients and their families with dignity and respect.
b) Considering the physical and emotional comfort of the patient as of paramount importance.
c) Using appropriate verbal and non-verbal communication to convey concern, pleasantness and professionalism to the patient.
d) Considering the patient’s modesty at all times.
e) Delivering health care services to patients without regard to race, ethnicity, religion, national origin, age, sex, gender, marital status, citizenship, sexual orientation, creed, disability, medical condition, socioeconomic status, political beliefs, or any status protected by law.
f) Not accepting gifts or gratuities from patients or their families.
g) Not engaging in sexual or romantic relationships with patients.
A professional appearance demonstrates respect for the PA profession, patients, campus, faculty, staff and self. Physician assistant students must dress in professional, neat and modest attire. Good personal hygiene is always required. Given the professional nature of the IU MPAS educational program in addition to the frequency of visiting guest lecturers and adjunct faculty, it is expected that students are appropriately dressed each day.
a) Requirements for All Didactic Experiences
1) Business casual is the preferred dress attire. Business casual attire must be worn during OSCE and patient encounters unless instructed by faculty.
2) Ceil blue scrubs blue are permitted during lectures and clinical skills labs. It is preferred that students wear a full set of scrubs (top and bottom), though IU MPAS apparel would be an acceptable choice on top.
3) Scrubs and a lab coat must be worn for gross anatomy lab.
4) No hats or head coverings except when associated with religious practice or for medical purposes.
5) Undergarments must remain unseen.
6) No body jewelry/piercing that interferes with class function.
7) No open-toed shoes during lab sessions.
8) No cologne or perfumes.
9) Hair should be worn in a manner that does not interfere when participating in clinical skills and patient care.
10) Dress requirements for physical examination laboratory sessions may be found in the respective course syllabus.
11) When required to be present at clinical sites, also observe guidelines below.
Faculty or staff who observe the violation of dress code are to send the student an email regarding inappropriate attire, cc the student’s advisor, and submit a professionalism incident report.
b) Guidelines for All Clinical Experiences
STANDARD A3.04The program must define, publish, make readily available and consistently apply a policy that PA students must be clearly identified in the clinical setting to distinguish them from other health profession students and practitioners.
1) Students must display prominently at all times their nameplate or embroidery on their white coat, which contains the student’s name and the title “Physician Assistant Student” (to be supplied by program), and respective hospital identification.
2) Professional dress is necessary for all clinical experiences.
a. Students will wear a clean, short white lab coat with program patch/embroidery and name plate/name embroidery.
b. Hair should be worn in a manner that does not interfere with clinical skills and patient care.
c. All attire will be clean.
d. Fingernails must be neatly trimmed. Artificial nails are prohibited.
e. No cologne or perfumes.
3) Any additional dress requirements imposed by a clinical site supersede those of the IU MPAS Program.
4) Scrubs should be worn in accordance with facility policy.
Students may use non-electronic earplugs in the classroom or during examinations. Electronic or noise-canceling devices are not permitted during examinations in accordance with standardized testing rules, unless otherwise directed by the Accessible Educational Services (AES).
Earplugs are subject to inspection prior to examination.
Physician assistant students must always maintain a professional and calm demeanor, even in emergency and other highly stressful situations.
Physician assistant students must comply with the University’s Drug and Alcohol Policy https://alcohol.indianapolis.iu.edu/know-laws/index.html#university-campus-policies and all other applicable policies and procedures concerning the use of drugs and alcohol at clinical sites. Students are prohibited from appearing at any clinical site while under the influence of alcohol or any drug that may affect performance or judgment. Students may be subject to random or required drug screening at the request of the clinical site facility. A positive drug screen will result in a professionalism review (see Section E: 14. Professionalism review), which may result in deceleration or dismissal from the program.
Attendance and timeliness are important aspects of professional behavior. Students must report to all classes, labs, seminars, end-of-rotation days, clinical sites and other scheduled activities on time. Timely return from designated breaks is required. Students must return messages from IU MPAS Program staff, faculty, clinical preceptors and clinical sites within 24 hours.
Students must submit all required assignments and forms on or before the designated date and/or time they are due.
Students should address principal faculty, the program director, the medical director, and others whom earned doctoral degrees as “Doctor”. It is at the discretion of the individual to permit students to use their first name instead of “Doctor”. Faculty with master’s degrees may be addressed by their first name. Adjunct faculty and guest lecturers should be addressed as they are introduced. During the clinical phase, faculty preceptors with doctoral degrees may permit students to address them by first name, consistent with clinical practice.
All IU MPAS students must complete criminal background checks and drug and alcohol screenings as directed by the program and as required by clinical rotation site affiliation agreements. As part of the matriculation process, students are required to obtain a background check. Additionally, students will be required to complete a second background check prior to the commencement of clinical rotations.
Additional screenings may be required at any time during the clinical year depending on the requirements of clinical affiliation agreements.
Additional screenings may be required at any time during enrollment in the IU MPAS Program at the discretion of the Student Progress Committee.
Students will be instructed on which company to procure the background checks. It is the student’s responsibility to log in and register for this important screen. It is also the student’s responsibility to pay the fee for these screens. Background check results must be sent electronically to the IU MPAS administrative coordinator or the designated online portal for the program to maintain these records.
A criminal background check that reveals any findings other than a minor traffic violation or positive drug and alcohol screening may negatively impact the student’s continuation in the program. Such cases will be referred to the Student Progress Committee for review.
Prior to Matriculation:
Students with positive findings on pre-matriculation background checks and screenings will be reviewed by the admissions committee to determine eligibility of matriculation into the IU MPAS Program, consistent with policies regarding professional behavior.
During Enrollment:
Students with new positive findings during enrollment from background checks or other screenings will be referred to the Student Progress Committee for review, consistent with policies regarding professional behavior.
Student must disclose arrests, formal charges, or convictions, other than minor traffic violations, within 2 business days of the offense. This must be submitted to the Program Director in writing. Student failing to report such offenses will be subject to immediate dismissal. Any report to the Program Director will be referred to the Student Progress Committee for review.
Other Considerations:
It is the student’s responsibility to ensure compliance with all health requirements and to ensure background checks are kept up to date.
The IU MPAS Program reserves the right to deny admission, prevent progression, or dismiss a student based on the results of a criminal background check or other screenings, or if a student refuses to participate in requested testing.
Clinical sites reserved the rights to refuse student participation based on such findings.
Graduation from the IU MPAS Program is not a guarantee of certification/licensure/registration as a physician assistant. If a student has a criminal history or history of drug and/or alcohol abuse, the student should consult with an attorney and/or the state licensing board to ensure that the student will be eligible for licensure.
Other Considerations:
It is the student’s responsibility to ensure compliance with all health requirements and to ensure background checks are kept up to date.
The IU MPAS Program reserves the right to deny admission, prevent progression, or dismiss a student based on the results of a criminal background check or other screenings, or if a student refuses to participate in requested testing.
Clinical sites reserved the rights to refuse student participation based on such findings.
Graduation from the IU MPAS Program is not a guarantee of certification/licensure/registration as a physician assistant. If a student has a criminal history or history of drug and/or alcohol abuse, the student should consult with an attorney and/or the state licensing board to ensure that the student will be eligible for licensure.
Failure to Disclose: Any failure to disclose a prior or new criminal charge or conviction at the time of application, matriculation, or during enrollment will be treated as a breach of professional conduct and may result in immediate dismissal from the program.
The IU MPAS Program reserves the right to immediately dismiss any student whose behavior is found to violate the values, ethical standards, or integrity of Indiana University or the PA profession.
Students should submit course/module and instructor evaluations for all courses. It is very important that students provide course/module and instructor feedback so that the program may use this information to make curricular changes and for faculty to improve upon their teaching. All responses are anonymous and will not be reviewed until final grades are assigned. The didactic education director and program director will monitor compliance with submission of evaluations for each course.
Students must continuously adhere to the IU MPAS Program’s professional behavior standards (as outlined in this handbook), the AAPA Guidelines for Ethical Conduct for the Physician Assistant Profession(https://www.aapa.org/wp-content/uploads/2017/02/16-EthicalConduct.pdf), <-- ( 3rd party pdfs linked on our site must still be accessible with new standards coming in 2027, not sure if this is. Found a link with some general info and gives the opportunity for download: https://www.aapa.org/career-central/practice-tools/ethical-guidelines-for-the-pa-profession/) and the IU Code of Student Rights, Responsibilities & Conduct (https://studentaffairs.indianapolis.iu.edu/student-conduct/index.html). Students who fail to meet these standards of professionalism and conduct are subject to professionalism review. If the transgression occurs related to a course (i.e. low professionalism competency on a preceptor evaluation or failure to turn in graded or ungraded assignments in a didactic course) the review process will follow the academic review process. If the transgression is not related to a course, then the review process will occur as below:
a) Students will receive a formal written communication from the IU MPAS Program Director notifying the student of a potential breech in conduct that was reported to the Program Director. It is at the Program Director’s discretion to meet with the student prior to disseminating the formal written communication about the professional misconduct.
b) Prior to the review process, the student involved will be asked to submit a formal written account of the alleged transgression in question, which must be completed within 7 days of notice from the Program Director
1) The Program Director will appoint a professionalism review ad hoc committee of at least three individuals, comprised of School of Health & Human Sciences faculty (which includes PA program principal faculty, instructional faculty, medical director, and program director). External individuals to the school may be considered to serve on the committee on a case-by-case basis. The ad hoc committee will review the evidence of the alleged transgression and will have the ability to listen to the student’s perspective as well as any other involved parties. The student has an opportunity to appear before the ad hoc committee prior to the recommendation of action. The ad hoc committee will determine the time and date of this meeting.
2) The ad hoc committee will report the findings to the PA faculty for a collective vote. A majority vote of PA faculty will determine the outcome of the Professionalism ad-hoc. The Program Director will notify the student of the finalized action plan within 7 days of the decision.
3) Recommendations may include but are not limited to a formal warning, remediation, or dismissal.
a. Action plans for remediation will include specific requirements of the student as well as a timeline for completion.
b. Failure to conform to the action plan will result in dismissal.
c. Reoccurrence of similar non-academic transgressions may result in further sanctions, including an immediate dismissal from the IU MPAS Program.
Timeline: While the timeframe for each step is noted to be 7 days, it is recognized that deadlines may need to be extended for good cause (i.e.: appeal forwarded during a holiday period or in the summer when faculty are not readily available). An extension for good cause should be communicated in writing (e-mail is acceptable).
Creating a collaborative learning environment is done with the intent of assisting the participants to achieve a better understanding of the course material and thus a more permanent knowledge to use when making clinical decisions. This environment should provide students with an excellent resource for test preparation, assignment completion, and effective practical exam performance.
Collaborative learning environments DO NOT constitute the following:
• Sharing of answers for assignments, exams, or papers.
• Providing others in your class or other classes with completed assignments, exams, or papers from previous years.
• Completing individual non-group assignments or papers together providing each other with answers to questions. We anticipate that you will discuss and reflect on assignments with peers, but the work submitted must be your own.
• Asking colleagues for specific information about test questions or detailed test content.
• Using someone else’s ideas and submitting it as original work. This is an example of plagiarism.
A violation of the collaborative learning environment in this way represents academic dishonesty and could result in dismissal from the program for all individuals involved. Thus, if you are ever unsure as to what is or is not acceptable collaboration, always discuss the situation with your course instructor, advisor, or department chair.
Article I: Section F
STANDARD B1.01The curriculum: c) includes core knowledge about established and evolving biomedical and clinical sciences and the application of this knowledge to patient care, d) provides the necessary breadth and depth to prepare students for the clinical practice of medicine
STANDARD B1.02The curriculum design reflects content and course sequencing that builds upon previously achieved student learning.
The courses offered by the IU MPAS program have been specifically designed and sequenced to prepare students to administer medical care to patients. According to the ARC-PA 6th Edition Standards, the program curriculum should prepare students “to work collaboratively in interprofessional patient-centered teams” and “to practice evidence-based medicine”.
Further, according the ARC-PA 6th Edition Standards the professional curriculum for PA education includes medical, behavioral, and social sciences; patient assessment and clinical medicine, social determinants of health, medical care of patients with special considerations, clinical reasoning and problem-solving, health across the lifespan, technical skills, basic counseling and patient education, evaluation of medical literature, business of health care, public health, patient safety, health policy, professional practice issues, medical ethics, personal wellness, and provider burnout; and supervise clinical practice experiences.
In accordance with the ARC-PA Standards and with the desire to graduate competent clinicians capable of delivering high quality health care, rigorous academic standards have been established for continued matriculation in the IU MPAS Program. Students are expected to complete all course assignments as outlined in individual course syllabi and to meet the IU MPAS Program academic standards as outlined in this manual (see Section G: Academic Policies). Students will be given updates to these standards as they occur.
Article I: Section G
Section G: Academic Policies
STANDARD A3.14The program publishes, consistently applies, and makes readily available to enrolled and prospective students: a) any required academic standards to maintain enrollment and progress in the curriculum, b) requirements and deadlines for completion of the program
Preparing for a career in the physician assistant discipline is a rigorous undertaking. Clinicians are expected to possess not only excellent clinical skills, but also to practice according to the highest ethical and professional standards. Preparation for meeting these high standards begins during a student’s education. Some students may occasionally experience academic difficulties. Such difficulties are best addressed early, before they grow to an unmanageable burden.
As clinicians, physician assistants are expected to exercise sound clinical judgment. As students, it is also important to exercise sound academic judgment and seek academic assistance when necessary. Students should consult with their course instructors, academic advisors, the Didactic Education Director, Clinical Education Director, or Program Director as soon as a difficulty becomes apparent.
This section outlines the academic performance expected of students in the IU Master of Physician Assistant Studies (IU MPAS) Program. It also describes the nature of the Student Progress Committee (SPC) and the procedures for submitting an appeal and addressing a grievance.
a) Grading Structure
The grading structure for all academic coursework, effective August 2020 follows the IU Indianapolis grading scale for the didactic courses and the S/F scale for the clinical year courses, though all course final grades must be passed with at least a “C” in order to progress during the didactic year and progress into the clinical year. Course final grades that are below a “C” will constitute a program course failure and the student will enter the course failure remediation policy for the respective phase of the program (didactic or clinical or program) depending on prior course failure, course remediation, or probation.
| Letter | Range | Point |
| A | 93–100 | 4.0 |
| A- | 90–92.9 | 3.7 |
| B+ | 87–89.9 | 3.3 |
| B | 83–86.9 | 3.0 |
| B- | 80–82.9 | 2.7 |
| C+ | 77–79.9 | 2.3 |
| C | 73–76.9 | 2.0 |
| F | <72.9 | 0.0 |
| I | Incomplete | |
| S/F | Satisfactory/Fail (clinical year courses) | |
| W | Withdrawal |
State Law Compliance for Satisfactory/Fail Courses
In accordance with Indiana law, the IU MPAS Program may only designate a course as Satisfactory/Fail if the determination of Satisfactory or Fail is based on the assessment of student’s ability to achieve course learning outcomes. Satisfactory/Fail status may not be assigned based on attendance, participation, or other non-merit criteria alone.
b) Temporary Grades
Due to extenuating circumstances, a student may earn an incomplete grade at the discretion of the Course Director. The student and Course Director will determine an appropriate plan and due date for incomplete work on an individual basis. Additionally, if a student takes a leave of absence in the middle of a course or if at the end of the semester the clinical preceptor evaluation is not yet available, then an incomplete would be appropriate.
c) Academic Standing
In order to progress through the program successfully, IU MPAS students are expected to complete the prescribed sequence of academic coursework and clinical rotations.
Didactic:
To remain in good academic standing, students must maintain a program cumulative grade point average (GPA) at or above 2.75. If a student falls below the 2.75 cumulative program GPA the student will be put on probation for one semester. The student must improve their cumulative program GPA to 2.75 by the end of the subsequent semester or the student will be dismissed from the program. In the event a student does not have a cumulative program GPA of 2.75 by the end of the fourth semester (end of didactic year) the student will be dismissed from the program as they will not be permitted to go on to the clinical phase while not in good academic standing.
Clinical:
To remain in good academic standing, students must improve their cumulative program GPA to 2.75 by the end of the clinical year. In the event a student does not have a cumulative program GPA of 2.75 by the end of the program, the student will be dismissed from the program.
GPA calculation will be deferred to the policy that is followed by the IU Indianapolis Registrar’s office.
Students will strive to successfully complete didactic coursework and clinical rotations for several reasons:
1) to remain in good academic standing,
2) to successfully complete the IU MPAS program and
3) to prepare for clinical competency and professional practice.
It is program policy that each didactic course must be passed witha grade of “C” or better.Any grade below this standard will be considered a course failure. |
Article I: Section H
Section H: Absence
Physician Assistant education is intense. In general, attendance is expected at all IU MPAS Program educational sessions, including clinical rotations. Enrollment in a physician assistant training program should be viewed as a job for 27-months. Employers both restrict time off and have policies in place to request absences.
Students should exercise sound judgment when making decisions regarding missed course lectures, assignments, exams, or clinical rotations. As such, it is imperative that students attend all scheduled classes and rotation shifts to maximize the experience during the limited time frame of the program. Each student is permitted five absences for each phase of the program, excluding bereavement, military duty, program requested days, prospective job interviews, or emergencies. Absences may not exceed more than two per semester during the didactic phase or two per each clinical rotation. An academic review will occur for any absences in excess of these policies.
Additionally, during the clinical phase, if more than two days of absence occur in a given clinical rotation (for any reason) the program will evaluate if the student is able to meet their competencies for that rotation in the time the student remains on the rotation or the ability to meet this competency in other rotations. The program will then determine if time needs to be made up to achieve those competencies and/or minimum requirements (for instance, minimum requirements and competencies for surgery will be difficult to achieve on any other rotation). This may require repeating a rotation in its entirety or remediating portions. This is a case-by-case basis that will involve the program director, clinical education director, and the respective faculty course director for the relevant clinical rotation(s).
Except for emergency situations approved by the program director, the following will not be permitted to be made up for credit: didactic in-person class assignments and assessments, end of rotation examinations, summative evaluation, clinical immersion week activities. For their own learning and as demonstration of professional behavior, students are expected to complete all required assignments that occurred during the absence, if feasible based on the type of assignment for no credit or feedback.
All absence requests must be submitted via the Canvas Absence Assignment listed in the cohort’s respective Canvas course. Additionally, the student must email either the Didactic Education Director or Clinical Education Director depending on their phase in the curriculum and the clinical education program assistant (who is monitoring absences) that they submitted the request. Approval or denial will be documented only in the submission comments. Students are to notify course directors/block directors and/or preceptors of their absence following approval and include a screenshot of the approval.
Approval will not be given for any lab or case-based class activities, including but not limited to patient evaluation lab, clinical skills labs, and clinical reasoning case days, except in extreme cases as determined by the course director or program director.
Below are details concerning the different type of absences.
Anticipated Absence:
• Religious observation- Requests for time off for religious observation must be submitted by the first week of the semester in which the religious observation occurs. Only the day of the religious observation will be approved for time off. This time off does count toward the total five absences for the phase of the respective program.
• Medical appointments- Students should make all attempts to schedule their routine medical appointments during the wellness block in the schedule in didactic phase and during days off in clinical phase. Absence for medical appointments count toward the maximum days off. Requests for time off must follow the above absence request process.
• Military duty- Time off to fulfill military obligations does not count toward the maximum days off permitted per phase of the program. Requests for time off for military duty must follow the above absence request process. Time off extending beyond two consecutive weeks must be discussed with the program director to determine if deceleration is appropriate.
• Bereavement- see bereavement policy (see 3. Bereavement). Requests for bereavement time off must follow the above absence request process.
• Program requested time away from rotation (i.e. prospective student interviews, representation at a conference, etc)- If a student is requested by the program to participate in events on behalf of the program, this absence will not count toward the three maximum absences allowed. The student must still follow the absence request process for documentation purposes.
• Prospective Job/Fellowship Interviews- As graduation nears, it is expected that students will miss rotation shifts to attend prospective job interviews. Requests for time-off for interviews follow the absence request process. Documentation of the interview will be required with the absence request. Students are permitted up to two days off for interviews per rotation in the spring and summer semesters and does count toward the maximum two days off per rotation policy. Prospective interviews will not count toward the maximum five days off for the clinical phase, however.
• Time off for personal obligations- The program understands students have important life events they want to attend while enrolled in the program. It is up to the student to determine the importance of attendance at these events as only five days per phase of the program and no more than two days off per semester or rotation is permitted, which includes time off for illness. Requests for time off must follow the above absence request process. For clinical phase, the absence requests must be made at least 30 days prior to the first day of the rotation.
Unanticipated Absence:
• Illness- Students must request time off for illness. Illness that requires absence of more than two days will require documentation from a licensed health care provider (provider must not have family relation to the student). In instances where a student is absent for three or more days during a didactic semester or a given clinical rotation and/or five days for the phase of the program, each subsequent time off for illness will require documentation from a licensed health care provider regardless of duration of illness.
• Emergency- There are instances in which true emergencies occur and a student will need time off. The program director will determine if the situation is extenuating to be consider an emergency. The student must provide the program director documentation of the emergency as soon as possible, preferably within 24-hours of the incident. The student must complete an absence form within 24-hours of the incident, if feasible. Emergencies will be evaluated on an individual basis and consideration for deceleration will be discussed when absence will extend beyond two weeks.
Unexcused absences (absences not approved) will result in an academic review (see Section I: Academic progress).
STANDARD B4.01The program conducts frequent, objective, and documented evaluations of student performance to ensure students meet the program’s learning outcomes for both didactic and supervised clinical practice experience components. The evaluations: a) align with what is expected and taught, b) allow the program to identify and address any student deficiencies in a timely manner
Students are required to be present for examinations as scheduled. Exams will begin at the scheduled time; students should arrive promptly to avoid disturbing other students and to take advantage of the allotted test time. It is at the instructor’s prerogative to administer a test to a tardy student after a classmate has already submitted their completed exam.
In the event of an emergency, documentation to support the necessity of the student’s absence will be requested. Approval to reschedule the exam will be determined on an individual basis by the program director.
Anticipated circumstances that warrant a rescheduling of an examination include presentation of a local or national conference which must be approved in advance by the program director.
It is the student’s responsibility to schedule the make-up exam with the faculty responsible for the exam. Make-up exams may be administered in either a paper, electronic or oral format. The format of the make-up exam will be determined by the instructor. Failure to take a rescheduled exam will result in a grade of zero (0%).
Absence from class or a clinical rotation will be granted for the death of a first-degree relative, grandparent, or other individual(s) deemed significant to the student. The student will typically be allowed up to 4 days for bereavement. The student should consult with the Program Director so that a plan may be put in place to allow the student adequate time for make-up work. Documentation of the death/services will be required.
Article I: Section I
STANDARD A3.14The program publishes, consistently applies, and makes readily available to enrolled and prospective students: a) any required academic standards to maintain enrollment and progress in the curriculum, b) requirements and deadlines for completion of the program, c) policies and procedures for remediation, d) policies and procedures for deceleration, e) policies and procedures for withdrawal, f) policies and procedures for dismissal
The IU MPAS Program and the School of Health & Human Sciences (SHHS) at Indiana University prepare students to become leaders in the health sciences. The role of the Student Progress Committee is to ensure that students meet both the program and school standards for:
• academic performance,
• clinical skills and
• professionalism.
It is imperative that students demonstrate progressive levels of competence throughout their educational journey, ensuring their readiness for clinical practice. Therefore, students must achieve an Advanced Beginner (Level 2) competency by the end of the didactic phase and Competent (Level 3) competency by the end of the clinical phase of the program. For additional minimum requirements related to PDAT competencies, please see PDAT appendix.
Monitoring and Support:
a) Regular monitoring of student progress will be conducted throughout both the didactic and clinical phases.
b) Students who demonstrate deficiencies in achieving the required competency levels will be provided with additional support, remediation, and resources.
c) Regular feedback and guidance will be provided to students to facilitate their progression towards competency.
d) Students who fail to achieve the required competency levels by the end of each phase may be subject to remediation, additional training, probation, or dismissal from the program.
e) Successful completion of remediation activities is necessary for progression to subsequent phases of the program.
STANDARD B4.01The program conducts frequent, objective, and documented evaluations of student performance to ensure students meet the program’s learning outcomes for both didactic and supervised clinical practice experience components. The evaluations: a) align with what is expected and taught, b) allow the program to identify and address any student deficiencies in a timely manner
The IU MPAS Program curriculum is rigorous and requires full commitment from both the students and the faculty. Thus, the program uses an “Incident Form” to identify students who may be experiencing academic or clinical difficulties and to offer help at the earliest possible time in the semester and in the curriculum.
The Student Progress Committee reviews each student’s performance regularly and at the end of each semester to a) identify student academic deficiencies and b) to determine the student’s eligibility for progress to the next semester. The committee makes decisions whether a student’s progress must be delayed and develops agreements for student remediation.
At the end of the program, the SPC recommends each student to the Program Director for graduation, based on successful completion of academic requirements and the summative evaluation.
The SPC analyzes aggregate student data related to attrition, deceleration, remediation and performance in didactic and clinical courses.
a) Composition of the SPC
SPC is comprised of a committee of IU MPAS Program principal faculty.
b) Referral of Students to the SPC
It is the duty of the faculty responsible for an assessment to notify the SPC chair immediately of any students who fail to meet the standards for academic performance, clinical performance or professionalism as outlined above.
c) SPC Meetings
The SPC will meet regularly, report and discuss at faculty meetings, and at the conclusion of each semester to review the academic records of students. The SPC will be notified of student semester and cumulative GPAs following the official grades posted to the University Registrar each semester. The SPC will also meet on an as-needed basis to address events arising during the semester.
In addition to regular student performance monitoring, the SPC reviews the academic progress of students who have:
1) failed a course (grade of less than 73%) within the current semester
2) failed a clinical rotation within the current semester
3) been placed on probation and/or
4) exhibited chronic or frequent absenteeism.
At the conclusion of each semester, the SPC Chair will forward to the SPC and the Program Director the name for each student who:
1) is presently on probation
2) has failed one or more courses including clinical rotations and/or
3) has exhibited chronic or frequent absenteeism.
Each student is assigned a Faculty Advisor. During faculty meetings, the SPC Chair reports on student progress which is monitored on a regular basis. Faculty also share reports on how their advisees are doing throughout the curriculum.
Students who are identified to be at risk will be contacted by the student’s Faculty Advisor who will address the concerns and offer resources. Faculty advisors and/or student will document the encounter according to advising protocol and documentation process.
Students may be referred to one or more of the following services as needed:
- Tutoring
- Adaptive Education Services
- Course Director/Instructor
- Faculty Advisor
- Counseling & Psychological Services (CAPS)
- Bepko Learning Center
- Failure to achieve a passing grade on a course assessment will trigger assessment remediation. Remediation activities are at the discretion of the course director and are defined in the course syllabus. Failure to demonstrate competency on reassessment activities may result in course failure.
- Expectations for remediation will be discussed with the student at the start of the assessment remediation.
- See course syllabus.
- See appendix T: Remediation Documents
STANDARD B4.01The program conducts frequent, objective, and documented evaluations of student performance to ensure students meet the program’s learning outcomes for both didactic and supervised clinical practice experience components. The evaluations: a) align with what is expected and taught, b) allow the program to identify and address any student deficiencies in a timely manner
NOTE: For Course Failure and Remediation in clinical phase, see Article II
a) When a student receives an end of course grade <73%, the course director will report the earned course grade to the registrar (i.e, C-, D+, D, D- or F). Specific course requirements to successfully pass a course with 73% or better are outlined in the respective course syllabi.
b) Students who earned 70%–72.9% will have two options for their remediation plan. The student will meet with both the Program Director and the student’s Faculty Advisor to discuss the options. Following the student’s decision, the Program Director will provide written documentation of the remediation plan. The two options are:
i) Completion of a four-week remediation assignment which would consist of self-directed studying culminating in a high-stakes multiple-choice examination including justification for their answer choices. When the final grade is determined not by a multiple-choice examination but rather a final project or paper, the student will be responsible for completing a project/paper based on similar concepts as the original project. The student may turn in completed work before the end of the 4-week remediation period. If the student fails to turn in the remediation assignment on time or at all, the student is considered to have failed two courses and is dismissed from the IU MPAS Program.
• Course remediation in the fourth semester must be completed prior to commencing the clinical phase and thus may result in a decelerated clinical year.
• If the student fails the remediation reassessment, the student will be dismissed from the program.
ii) Decelerate into the subsequent cohort and repeat the entire curriculum including the semester in which the course failure occurred. Students must re-enroll in the courses and will be responsible for the cost of the repeated courses. All courses must be completed with a “C” or better. Calculation of the student’s cumulative GPA will be deferred to the campus policy. If the student earns <73% in any repeated courses this constitutes a second course failure and is grounds for dismissal.
• If the student earns <73% in any repeated courses this constitutes a second course failure and is grounds for dismissal.
c) Those who earn <70% in one course will only have the option to decelerate into the subsequent cohort and repeat the curriculum as outlined above.
General remediation information:
The course failure, even if successfully remediated, counts toward the maximum number of two course failures as grounds for dismissal (see 11. Sanctions). Thus, if a student fails a subsequent course they will be dismissed from the IU MPAS Program.
A student with two or more course final grades below “C”, which is a course failure by program definition, in one semester will be dismissed (see 11. Sanctions) from the program, without an opportunity to remediate.
Academic reviews are intended for students that a) fail to meet the standards of professional conduct as part of a course (i.e. low professionalism competency on a preceptor evaluation or failure to turn in ungraded assignments in a didactic course) or b) are at risk to fail a course due to not meeting course requirements.
The review will be conducted by an ad hoc committee of the program director, the respective course director and either the clinical education director or didactic education director depending on the student’s phase of the curriculum. Should any of these individuals hold more than one role for a particular student’s case, the Student Progress Chair will step in to one of the roles.
The ad hoc committee will review all documentation and evidence regarding the respective incidence (professionalism transgression or academic course failure) within 7 days of notification to the program director. At the discretion of the committee, the student may be requested to provide additional written or verbal narrative regarding the transgression before an action plan is determined. The ad hoc committee will determine the action plan and present this action plan to the PA faculty for a vote. A majority vote will be the deciding factor. This action plan will be disseminated via written documentation to the student within 7 days following review by the Program Director. As this is an academic review, the student may submit an appeal per the appeals process.
Timeline: While the timeframe for each step is noted to be 7 days, it is recognized that deadlines may need to be extended for good cause (i.e.: appeal forwarded during a holiday period or in the summer when faculty are not readily available). An extension for good cause should be communicated in writing (e-mail is acceptable).
Deceleration refers to a disruption in a student’s academic progress of two weeks or more. If a student encounters medical and/or personal difficulties which would keep the student from continuing in the program for more than two weeks, and if the student is not concurrently being considered for dismissal, the student may petition the Student Progress Committee (SPC) via the Program Director and the student’s Faculty Advisor for a leave of absence and deceleration of progress.
Students must be in good academic standing (minimum 2.75 cumulative program GPA) to be considered for deceleration and readmission into the program.
• The student must meet with the Program Director prior to submitting the petition for leave.
• The student’s written request for a leave of absence must include reasons for the request, and the amount of leave time desired, including estimated return date.
◦ If a leave is taken for medical reasons, the program will require certification from a licensed healthcare professional attesting to the student’s fitness to resume coursework and the ability to meet technical standards.
• Each situation will be evaluated on an individual basis through a SPC review committee to make a final disposition on the leave request.
◦ A student may appeal the SPC review committee decision by submitting a formal request to the Department Chair within 7 days of notification of the SPC disposition, who will then convene an ad hoc appeal committee consisting of three faculty from SHHS graduate professional programs. The SHHS ad hoc appeal committee has 7 days to review the appeal and provide a response to the Department Chair.
Granting of a leave of absence does not imply full or partial refund of tuition and/or fees. Any potential refund is subject to University policy.
All didactic courses in the IU MPAS program are offered only once an academic year and serve as prerequisites for subsequent courses, thus, the student will continue the didactic portion the following year. During the clinical phase, a returning student’s remaining clinical rotation assignment(s) will be made based on clinical site availability.
Students must abide by the continuation procedure as outlined in the next section
The IU MPAS program is committed to maintaining low attrition rates while ensuring timely completion of the program. In alignment with this commitment, the program defines a completion timeframe of 60 months from the start of the program which aligns with the IU Graduate School policy. This timeframe serves as a guideline to ensure students’ progress through the curriculum efficiently while maintaining time for personal or medical leaves. The program recognizes the importance of timely completion for students' career advancement and the overall success of the program.
Leave of absences during didactic phase: A student who has been granted leave from the IU MPAS Program during the didactic phase must notify the Program Director of their continuation in the program at least ninety (90) days prior to the start of the semester for which they anticipate their return.
Leave of absence after completion of didactic phase: A student who has been granted leave from the IU MPAS Program following completion of the didactic phase must notify the Program Director of their continuation in the program no less than one week prior to the start of their next scheduled clinical rotation.
For leave of absence due to medical reasons: the Program Director will require documentation from a health care provider that the student is able to return to the program and meets the program’s technical standards. The student will also be asked to sign the attestation that they currently meet the technical standards.
At the time of leave, it is the student’s responsibility to arrange in writing a continuation agreement with the IU MPAS program through the Student Progress Committee.
• The student is allowed to resume academic progress as specified in the continuation agreement.
• The student must meet any specific academic requirements associated with resuming coursework under the continuation agreement.
• Students failing to abide by the continuation agreement are subject to dismissal from the School of Health and Human Sciences.
Students choosing to withdraw from a course (not including leave of absence) or from the program due to a failing grade will not be permitted readmission into the program.
Students who withdraw will be subject to the current University policy at IU Indianapolis.
Students who fail to meet the academic standards outlined by the program may be subject to academic sanctions including establishment of a learning contract, probation, suspension and/or dismissal. Students who are not in good academic standing or on suspension may not participate in Graduation ceremonies.
a) Probation
Students who are on probation will be referred to the Student Progress Committee for evaluation and development of an action plan.
Grounds for being considered for placement on probation include, but are not limited to:
• failure to maintain Good Academic Standing (Good Academic Standing is defined as: =2.75 cumulative GPA during didactic phase),
• course failure,
• =3 exam failures within one semester,
• =5 exam failures within one phase of the program (i.e. didactic or clinical),
• academic misconduct, and/or
• lapse in professionalism (i.e.: non-academic misconduct).
Students have the ability to be considered for removal from probation by the Student Progress Committee based on the action plan. In addition, students may be removed from probation at end of the didactic phase based on demonstration of competency. This will be determined by SPC.
b) Suspension
In the event that a student poses a danger to themself, faculty, staff or patients, the student may be suspended until the situation is investigated or the student is dismissed from the program. Suspension may result in deceleration from the program and would follow the readmission procedure (see 10. Academic Withdrawal).
c) Dismissal Policy
Grounds for dismissal include but are not limited to any one of the following:
1) two (2) course failures
2) failure to meet good academic standing GPA after one semester of probation
3) failure to meet good academic standing GPA at the conclusion of the fourth semester prior to progression to the clinical year
4) failure to meet conditions established in a course remediation agreement
5) failure on the Summative Evaluation Remediation reassessment
6) demonstrated lapse in professionalism and/or
7) academic dishonesty.
A student who has been dismissed will not be eligible to reapply for admittance into the IU MPAS program at any future time.
The IU MPAS Program reserves the right to immediately dismiss any student whose behavior is found to violate the values, ethical standards, or integrity of Indiana University or the PA profession.
The IU MPAS curriculum is a 27-month program. The curriculum is composed of seven consecutive semesters, divided into a didactic phase (15 months) and a clinical rotation phase (12 months).
For a student to progress through the program and graduate from the IU MPAS program, they must meet the following requirements:
1. Earn a course grade of C or higher in each course during the didactic phase. In case of course failure, a) the remediation independent study course must be passed with a grade of C to complement the course grade below C in the original course to be eligible for graduation, or b) all the repeated courses earn at least a C. The required didactic courses are listed below.
a. ANAT D528, MPAS M500, MPAS M501, MPAS M502, MPAS M503, MPAS M504, MPAS M505, MPAS M506, MPAS M507, MPAS M508,
MPAS M509, MPAS M510, MPAS M531, MPAS M532, MPAS M694, MPAS M696, MPAS M818
2. Earn a course grade of “S” or Satisfactory in each course during the clinical year phase.
a. MPAS M681, MPAS M682, MPAS M683, MPAS M684, MPAS M685, MPAS M686, MPAS M687, MPAS M 688, MPAS M689, MPAS M690,
MPAS M691, MPAS M695, MPAS M697, MPAS M698, MPAS M700
3. Maintain a cumulative GPA of 2.75 or above to be in good academic standing during the didactic phase. Students must have a cumulative GPA of 2.75 or greater to progress to the clinical year phase.
4. Satisfactorily demonstrate clinical rotation competencies earning at minimum a “Satisfactory” grade in all clinical rotations
5. Complete the PACKRAT self-assessment in both the didactic year and clinical year phases.
6. Complete the clinical year competency checklist demonstrating proficiency in all areas.
7. Complete all clinical minimum patient encounter requirements.
8. Earn a passing grade on all components of the summative evaluation, demonstrating achievement of a level 3 (competent) in all IU MPAS competencies.
9. Complete a minimum of one professionalism self-assessment during both the didactic year and the clinical year.
10. Complete the competency survey, exit survey and focus groups during the final month of the program.
Students will undergo two reviews: (1) a progression review prior to commencing clinical rotation to establish they have met all requirements to progress to the clinical year and (2) a graduation eligibility review within the last month of the program to establish they have met all program requirements to graduate.
Article I: Section J
STANDARD A1.02 The sponsoring institution is responsible for: g) defining, publishing, making readily available, and consistently applying to students its policies and procedures for processing student allegations of harassment and mistreatment
STANDARD A3.14 The program publishes, consistently applies, and makes readily available to enrolled and prospective students: g) policies and procedures for student grievances, h) policies and procedures for student appeals
Academic standards exist at the school, department and program level. To be eligible to appeal an academic standard or decision, the individual must be a student enrolled and/or taking coursework in the School of Health & Human Sciences (SHHS). A student has a right to appeal any decision concerning academic standards and decisions.
• Individuals appealing academic decisions are required to have a meeting with the course director prior to initiating a formal appeal.
• It is also recommended that the student meet with their academic advisor at this point. If the student's academic advisor is also the course instructor, then another faculty advisor may be assigned in consultation with the program director and the student.
Complaints that are either a) filed under or b) in active consideration by a University campus committee will not be heard by the program, department or school. Actions on academic misconduct and disciplinary matters proceed according to the campus specific policies and procedures, available at the following link: https://studentaffairs.indianapolis.iu.edu/student-conduct/index.html
During the appeals process, the student involved in the appeal may continue to attend classes but is not allowed to proceed with clinical rotations.
The procedures for an individual to formally appeal academic standards and decisions are presented in a flowchart format.
Routes for Appeal
There are three distinct routes a student may initiate a formal appeal of an academic decision.
I. Course Grade Appeal: Initiated at the course director level when a student wishes to contest a grade for an individual course, including sanction for academic dishonesty and/or final course grade.
II. Department/Program Dismissal: Initiated at the department/program level when a student contests dismissal or delay.
III. Review of Department/Program Dismissal: Initiated at the school level when a student is contesting the decision of the program or department to dismiss the student for failing to meet academic standards.
I. Course Grade Appeal:
A. Student initiates appeal if they want to appeal a course grade decision.
1. The student submits a letter of appeal to the course director within 7 days of the course director’s decision addressing each of the following:
a. The course academic standard or requirement being appealed.
b. The specific reason(s) for the appeal
c. Steps which were previously taken to meet the standard(s) or requirement(s).
2. The student should append the appeal letter with any additional documentation to verify and support the appeal.
3. The course director has 7 days to respond formally in writing to the appeal.
B. Program Director responsibilities
1. If the student is not satisfied with the course director’s decision, the student may appeal to the program director. If the course director is also the program director, the appeal shall be presented to the department chair.
2. Upon receipt of the student appeal, the program director has 7 days to review the appeal and to make a decision.
3. The program director is required to make a decision on the appeal based on the merit of the appeal. The program director may choose to consult with the student and the course instructor/director.
4. The program director is responsible for documenting their decision and justification including completion of Section I of the Appeals routing form.
5. The program director must respond to the student in writing on the outcome of the appeal.
6. In the event the decision of the program director is to uphold the student's appeal, the course grade will be adjusted accordingly.
7. In the event the decision of the program director is to deny the student's appeal, the course grade will be upheld. There are no further appeal options following this decision.
II. Program Dismissal Appeal
A. Student initiates appeal if he/she wants to appeal a program dismissal or delay.
1. The student submits a letter of appeal to the chair within 7 days after dismissal or delay, addressing each of the following:
a. The program academic standard or requirement being appealed.
b. The specific reason/s for the appeal.
c. Steps which were previously taken to meet the standard/s or requirement/s.
d. Projected steps which might be taken to meet the standard/s or requirement/s in the future.
2. The student should append the appeal letter with any additional documentation to verify and support the appeal.
B. Program Director responsibilities
1. Upon receipt of the student appeal, the program director has 7 days to review the appeal and to convene department faculty to determine merit of the appeal.
2. The faculty may request to interview the student or other involved parties. After reviewing the appeal, the faculty will vote to either uphold or deny the student's appeal. The chair will cast the deciding vote in the event there is a tie.
3. The program director is responsible for documenting the program’s decision and justification including initiation of the Appeals Routing Form.
4. The program director must respond to the student in writing on the outcome of the appeal at the department/program level within 7 days of receipt of the student appeal.
5. In the event the program’s decision is to reverse the initial decision, then the student's appeal is upheld, and the corrective action is initiated.
6. In the event the program does not overturn the decision and the appeal is denied, the student is entitled to take their appeal to the department level to request a review of the program decision. The program director must forward the original appeal packet and the Appeals Routing Form to the chair of the SHHS Department of Graduate Health Professions.
III. Review of Program Dismissal Appeal
A. Student initiates appeal at this level if they are dissatisfied with the appeal outcome at the Department/Program level (II).
1. The student submits a letter requesting review of the program’s decision to the SHHS Dean within 7 days of the program decision. The following information must be included with the request:
a. the original appeal packet that was submitted to the program; and
b. any additional pertinent documentation.
B. SHHS administrative office responsibilities
a. Upon receipt of the student appeal at the SHHS administrative office, the Dean for has 7 days to:
a. confirm student status in the SHHS;
b. provide consultation to the student and program regarding the appeal and the process.
c. If after consultation the student chooses to continue the appeals process, the Dean will then form an ad hoc student appeals committee and appoint a committee chair.
b. The student appeals committee will be composed of three tenured or long-term contract faculty within the SHHS but outside of the student's program.
c. The appeals committee has 7 days to review the appeal and complete a written report. To facilitate review of the appeal, the appeals committee may interview the student or other involved parties and request any additional information that would assist the committee in their decision.
d. The Appeals committee completes Section 2 of the Appeals Routing form.
e. The Dean receives the appeals committee’s recommendation and renders a decision within 7 days of receiving the recommendation and completes Section 3 of the Appeals routing form. The Dean then informs the student, the program, and the members of the appeals committee of the decision. The final copy of the original Appeals Routing form and all supporting documents are kept on file in the SHHS administrative office, with a copy provided to the program.
f. The final decision in matters related to the program or academic policy rests with the School of Health & Human Sciences Office of the Dean.
a) University Legal Counsel
The appeals committee may seek consultation with University counsel at any time during the appeal and decision-making process.
b) Timeline
While the timeframe for each step is noted to be 7 days, it is recognized that deadlines may need to be extended for good cause (i.e.: appeal forwarded during a holiday period or in the summer when faculty are not readily available). An extension for good cause should be communicated in writing (e-mail is acceptable).
c) Additional Student Rights
1. During the appeals process, the student involved in the appeal may continue to attend classes but is not allowed to proceed with clinical rotations.
2. If the student is requested to attend an interview at any level of the appeals process, he/she may bring an advocate to the appeals committee hearing who may be present and may advise the appellant during the hearing process. The advocate shall not be considered a party to the process and may not participate directly in the process.
In the event that the student's advocate is an attorney, the attorney may be present and advise the appellant but is not permitted to participate directly in the process (i.e. they may not speak on the appellant's behalf). Additionally, the student is required to give the Appeals Committee five (5) days’ notice to allow SHHS to have a representative of University counsel present during the appeal hearing. If the student fails to give the five (5) day notification required to have a legal representative present, the interview/hearing will be postponed.
STANDARD A1.02 The sponsoring institution is responsible for: g) defining, publishing, making readily available, and consistently applying to students its policies and procedures for processing student allegations of harassment and mistreatment
STANDARD A3.14 The program publishes, consistently applies, and makes readily available to enrolled and prospective students: g) policies and procedures for student grievances
a) Conditions for Presenting a Grievance
Students may address the SPC if they want to:
1) submit a grievance against a faculty/staff member
2) submit a grievance against a clinical supervisor and/or
3) submit a grievance against another student.
b) Grievance Procedure
In order for a grievance to be heard by the SPC, students should take the following actions:
1) Attempt to resolve the issue with the party resulting in the alleged grievance.
2) Attempt to address the matter with the Program Director when a satisfactory resolution cannot be reached by both parties.
3) Submit the Request to Present a Grievance or Appeal to SPC form to the Chair of the SPC when you cannot resolve the matter at the Program level, or if the matter directly involves the Program Director. This form should be submitted within 7 days of determining that the grievance cannot be addressed at the program level.
In the event that a student has not taken the above steps, the SPC will refer the student back to the individuals involved to attempt to resolve the matter.
c) Referral of Grievance
In some circumstances, the SPC may determine that it is not the appropriate authority to address a grievance. Should this be the case, the Chair of the SPC will work with the Program Director or the Office of the Dean to refer the case to the appropriate authority.
d) Report of SPC Findings
The SPC seeks to address appeals, grievances and review the performance of all referred students in a timely fashion. However, in many cases it will be necessary to review the situation in detail with the parties involved. After the case has been discussed to the satisfaction of the SPC, the SPC will forward written recommendations to the Program Director. In cases involving the Program Director, the recommendation will be forward to the Office of the Dean.
e) Additional Remedies
Students may have additional rights outside of the IU MPAS Program and the School of Health and Human Sciences. For a complete understanding of these rights students should refer to the IUI Code of Student Conduct at https://studentaffairs.indianapolis.iu.edu/student-conduct/index.html
Article I: Section K
As you progress through your education, it is important that you pay attention to your own health. Proper nutrition, sleep, exercise and stress-coping skills will contribute to your success as a student.
STANDARD A1.02 The sponsoring institution is responsible for: e) documenting security and personal safety measures for PA students, faculty, and staff in all locations where instruction occurs
IU MPAS defers to the campus security and safety measures and to clinical site security and safety measures. These are documented on the IU Indianapolis website and within clinical rotation affiliation agreements on file.
STANDARD A1.04 The sponsoring institution provides academic support and student services to PA students that are equivalent to those services provided to other comparable students of the institution.
STANDARD A3.06 The program publishes, makes readily available, and consistently applies policies that preclude the program director, medical director, and principal faculty from participating as healthcare providers for students in the program, except in emergency situations.
Although the Medical Director and the majority of program faculty and clinical preceptors are healthcare providers, they are not permitted to play any role in the evaluation or treatment of students including giving health advice to students.
IU Indianapolis Campus Health Services provides health services and education, treating each individual with respect and dignity.
Student Health Services, IU Indianapolis Campus Health
https://studentaffairs.indianapolis.iu.edu/health/medical/index.html
Lockefield Village, first floor
980 Indiana Ave Indianapolis, IN 46202
Student Appointments: 274-8214
Fax: 274-7657
STANDARD A3.07 The program publishes, makes readily available, and consistently applies written procedures that ensure timely access and/or referral of students to services addressing personal issues that may impact their progress in the PA program.
IU Indianapolis Counseling and Psychological Services (CAPS) promotes overall health and well-being by helping students overcome obstacles that may otherwise prevent them from attaining academic, personal and professional goals. It is the mission of CAPS to provide direct professional psychological services, including crisis response, counseling, assessment and referral that are accessible to, and provide for, the general well-being of all IU Indianapolis students.
CAPS provides year-round counseling, consultation, group counseling, relationship counseling and referral services to the IU Indianapolis community. Current fees for consultation and ongoing counseling can be found: https://studentaffairs.indianapolis.iu.edu/health/counseling-psychological/fees.html
Program faculty may refer students for counseling at any time if faculty feels students could benefit from counseling services. Students may also seek help on their own at any time. Students seeking counseling are encouraged to call to set up an appointment at 317.274.2548. Students may also stop by in-person and request to meet with a counselor.
Offices are located at 980 Indiana Ave Second Floor, Indianapolis, IN 46202. The offices are open Monday - Friday, 9am - 4pm. Limited evening hours are available by appointment only Tuesday/Wednesday/Thursday.
For more information go to: https://studentaffairs.indianapolis.iu.edu/health/index.html
If you believe someone is at immediate risk of harm to themselves or another, CALL the IU Indianapolis Police at (317) 274-7911 or your local emergency services at 911 or their local number.
If the individual is not at immediate risk, but expresses thoughts of harming themselves or another:
• Encourage the person to come to CAPS. Go to:
• https://studentaffairs.indianapolis.iu.edu/health/counseling-psychological/index.html to learn about when and how to refer.
• Consider contacting one of the 24-hour crisis phone lines:
◦ Crisis & Suicide Hotline at 317.251.7575
◦ Midtown Mental Health Center (24 hours) at 317.880.8485
It is mandatory that all IU MPAS students have health insurance coverage annually. Up to date Proof of Coverage must be submitted to the SHHS Director of Student Engagement and Success prior to matriculation. Once enrolled, Indiana University provides a student health insurance option. All students must demonstrate they have equivalent or better coverage in order to waive the student health insurance plan. Students annually will need to waive the student health insurance by the deadline or the student will be charged for the insurance on their bursar account. Students will be required to provide documentation of insurance each January for coverage during the respective academic year.
STANDARD A3.18 Student health records are confidential and not accessible to or reviewed by program faculty or staff, except for immunization and screening results, which may be maintained and released with the student's written permission.
STANDARD A3.09 The program publishes, makes readily available to current and prospective students, and consistently applies policies based on current CDC health professionals’ recommendations and applicable state or country mandates for: a) minimum immunization and health screening of students, b) international travel (for programs offering international curricular components)
Participation in an educational program preparing students to become health care practitioners may expose students to potential health risks, including hepatitis and HIV. The use of universal precautions by all students minimizes that risk. In addition, for the safety of students and patients with whom students might come in contact, all students in the IU MPAS program must have up-to-date vaccinations or provide proof of immunity by serum titers.
Students must:
a) Be fully immunized for: tetanus/diphtheria/pertussis, polio, hepatitis B, (measles), mumps, rubella, varicella, and meningitis.
b) Have tuberculosis screening each year.
c) Have an annual influenza vaccination.
d) Provide the IU Indianapolis Student Health Services with a copy of the student’s completed immunization form before attending new student orientation. Students are required to maintain a copy of their proof of immunizations to present at clinical rotation sites. Some clinical sites require students to directly provide proof of immunization and do not permit the program to send the information.
a. Written consent for the IU MPAS program to maintain a copy of the immunization records, annual tuberculosis screening test and annual influenza vaccination to provide to clinical sites will be requested of all students. If a student does not grant consent, then it is the student’s responsibility to provide proof of immunizations to the clinical rotation sites.
Full details on the procedure and requirements for each of these vaccinations are provided prior to the beginning of classes. It is the student’s responsibility to be fully current and immunized on all items listed above before entering any program or clinical situations. Failure to do so will result in the student being removed from the activity for the student’s own safety as well as that of other students and patients and will have a decelerated program completion date.
At any time, a clinical site may require additional immunizations to rotate through their site; students may have a delay in graduation if they are unable to comply with the clinical site required immunizations.
Should the university enact a new immunization requirement due to public health emergency, the department will follow the university immunization policy.
See Immunization for the complete list of immunizations required.
STANDARD A3.05 The program publishes, makes readily available, and consistently applies policies addressing student exposure to infectious and environmental hazards before students undertake any educational activities that would place them at risk. Those policies: a) address methods of prevention, b) address procedures for care and treatment after exposure, c) clearly define financial responsibility
Accidents may occur in the classroom or in the clinical setting. If a student is injured in a classroom setting, notify the instructor immediately. If a student is injured at a clinical site, the student should notify the clinical preceptor immediately and follow the site’s protocol for dealing with injuries. In many facilities, this will require students to seek treatment in employee health department, the occupational medicine department or the emergency department. If the clinical site lacks these resources, treatment should be sought at the nearest emergency department.
Exposure to blood-borne pathogens is a risk assumed by all healthcare providers. Students will be provided a refresher training prior to the start of clinical rotations. Individual clinical sites may also provide orientation sessions regarding blood-borne pathogens. Observing universal precautions is one method to reduce risk.
The principle of universal precautions recognizes that any patient may be infected with microorganisms that could be transmitted to other persons. Of particular concern are the primarily blood-borne pathogens HIV (human immunodeficiency virus) and HBV (hepatitis B virus). However, body fluids other than blood, secretions and excretions are included in universal precautions. Since infected patients may be asymptomatic, it becomes necessary to use basic precautions with every patient. Observance of universal precautions will help to provide better protection for every staff member. Students should also familiarize themselves with specific hospital and/or clinical site policies regarding universal precautions.
a) Universal Precautions Guidelines:
1) Act as though all patients you have contact with have a potentially contagious blood-borne disease.
2) Avoid direct contact with: blood, body fluids, secretions, excretions, mucous membranes, non-intact skin and lesions.
3) Avoid injuries from all “sharps” (i.e.: needles, glass vials, blades, microscope slides, etc.)
4) Avoid direct contact with items, objects and surfaces contaminated with blood, body fluids, secretions and excretions.
5) Dispose of all “sharps” promptly in special puncture resistant containers.
6) Dispose of all contaminated articles and materials in a safe manner as prescribed by law.
7) Wash hands frequently and thoroughly, especially if they become contaminated with blood, body fluids, secretions and excretions; and,
8) Use appropriate barriers, including: gloves, gowns, aprons, caps, shoe covers, leggings, masks, goggles, face shields and equipment such as resuscitation devices. These barriers are to be used to protect:
a. skin - especially non-intact skin where there are cuts, chapping, abrasions or any other break in the skin; and,
b. mucous membranes - especially eyes, nose and mouth.
9) Wear protective equipment as directed by the student’s clinical preceptor or facility protocol.
10) Follow bagging protocol before transporting specimens to the laboratory.
In the event that a student is injured by a contaminated sharp object or is exposed in any manner to blood or potentially infectious body fluids in the course of their assigned clinical work, the following steps should to be followed for proper treatment and follow up.
1) Upon possible exposure to a blood-borne pathogen
a. For skin and wounds, wash the affected area with soap and water. Eyes and mucous membranes should be copiously flushed with water. Notify your Clinical Preceptor immediately.
b. Follow facility protocols regarding evaluation. Most facilities will require you to report immediately to employee health or the emergency department following exposure. Failure to follow up properly may make it difficult or impossible to obtain source patient blood.
c. In sites without employee health or emergency departments, or if the site protocol is unclear, proceed immediately to the nearest emergency department for assessment as soon as possible.
d. The treating healthcare professional will request information about your medical history, the source patient’s history (if known) and the nature of the exposure. They may request to draw baseline laboratory studies. They will discuss your risk of contracting a blood-borne disease and the risks and benefits of prophylactic treatment. In deciding whether to receive post-exposure prophylactic treatment, students might also wish to consult with the National Clinicians Post-Exposure Prophylaxis Hotline: 888-HIV-4911 (888-448-4911).
e. Students should follow up as directed by their treating healthcare provider. Ongoing follow up may take place at the initial treating facility or the student may be referred to a healthcare provider with expertise in infectious disease.
f. Since a student is neither an employee of Indiana University nor an employee of the clinical site, payment for assessment and treatment is the responsibility of the student.
All students who experience an injury or exposure must complete an incident report and submit it to the IU MPAS Program Director and Clinical Education Director as soon as possible. Students should not delay prompt evaluation and treatment in order to complete paperwork. Evaluation and treatment are of primary importance.
During the COVID-19 pandemic, students with possible coronavirus (SARS-CoV-2) exposure or symptoms should follow the most recent guidance for IU Health.
As outlined in its international mission statement, the School of Health & Human Sciences (SHHS) is “committed to preparing students to live and work in a globally interconnected world by fostering and assisting faculty and students to enhance their international educational experiences”. We recognize that there are multiple opportunities for our professional healthcare students to travel abroad and believe that the benefits of participating in these experiences must be balanced with the risk of harm. We acknowledge that when our healthcare students participate in these activities, even if they are not sponsored by IU, there is the perception that the students are representing their healthcare professions as well as the University just by virtue of being professional healthcare students at IU.
In addition to safety concerns with regard to travel abroad, an appropriate student experience must account for the limited fund of knowledge and clinical skills possessed by the average professional healthcare student. Therefore, if the student will be participating in care delivery, the student must be supervised by a qualified healthcare professional. In order to promote the concept of a high quality international professional healthcare education experience that appropriately balances benefit and risk, the following policy outlines the process and expectations for such international experiences.
Scope of the Policy
Groups of SHHS students
This policy applies to all groups (i.e. more than one SHHS student) of SHHS professional healthcare students pursuing international educational opportunities whether organized, sponsored or arranged by SHHS faculty, staff, student groups or others as well as all individual SHHS professional healthcare students pursuing international educational opportunities where the student(s) are expecting or intending to observe, support or participate in clinical activities or care delivery. This policy will apply during scheduled academic semesters and during break periods. Applying this policy broadly to all SHHS professional healthcare student international travel opportunities ensures that there will be a thorough and consistent application of the relevant rules, procedures and other considerations.
• All international service-learning activities must be approved in advance by Indiana University's Overseas Study Advisory Council (OSAC).
• It is recommended that the OSAC process be started 12-15 months before the intended departure date of the students. Under special circumstances, the process may be expedited. Details of the proposal process are available at: https://overseas.iu.edu/policies/program-dev/proposals/guidelines.html
The OSAC process requires demonstration of support from the SHHS Dean's Office. Therefore, all such proposals must be provided to and approved by the SHHS Associate Dean for Academic and Student Affairs before submission to OSAC. After approval by the SHHS Associate Dean, the student group will then work with the IU Indianapolis Director of Study Abroad in the IU Indianapolis Office of International Affairs. That office will provide information and will route the proposal through the OSAC approval process. The Director can be reached at abroad@iu.edu or 317-278-0716.
When considering the development of an international experience it is important to know whether the destination country is under a US Department of State travel warning (not alert). For the list of travel warnings please see https://travel.state.gov/content/passports/en/alertswarnings.html. IU has a policy that it does not support student travel to countries under travel warnings. Details of this policy are available at https://overseas.iu.edu/policies/safety-responsibility/index.html. It is possible to request an exemption to the IU travel warning policy. Exemptions require approval by the Safety and Responsibility Committee of the OSAC. Decisions for exemptions will be based on the nature of the travel warning, including the locations most impacted by the warning, the experience and training of program organizers and local support staff, the importance and academic relevance of student involvement, what the program will do to minimize the risk to students, the extent of the safety and security orientation provided and the program's willingness to get the students' informed consent regarding participation, despite the travel warning.
When applying for approval, please use the SHHS pre-departure form:
Individual Students Pursuing International Activities
Processes for students who arrange their own individual international educational opportunities for academic credit are the same as the process for groups of students delineated in the previous section.
There are also instances in which individual SHHS professional healthcare students pursue international opportunities where the student is expecting or intending to participate in clinical activities or care delivery.
As long as the student is not receiving academic credit for such an activity and is not representing his or her program, school or the university, neither the program nor the school nor the university is involved in sanctioning these activities
When applying for approval, please use the SHHS pre-departure form.
Article I: Section L
Section L: Communication
According to University policy, the IU email address assigned to the student at time of enrollment is to be used for official communication and the student is responsible for all communications so sent. Students are reminded that University email should reflect civil discourse.
When enrolled in a class in which the CANVAS platform is utilized, students are reminded that when they are requested to use the forum or discussion applications, postings should reflect civil discourse. Also, since these postings can be viewed by others in the class, students should be mindful of HIPAA regulations and maintain confidentiality when discussing a case or a patient situation.
While personal email, social media accounts and other forms of electronic communication are the purview of the individual, students should be mindful that their comments may be interpreted in the context of a graduate student at IU. Students should be particularly alert not to violate HIPAA regulations even in personal correspondence.
Students must not add faculty, staff, or preceptors to social media while enrolled in the program. Connecting with faculty and preceptors through LinkedIn is permissible for professional purposes only while students are enrolled in the program.
Should students appear to violate HIPPA regulations or appear to misrepresent the values of the program on social media, a professionalism review will be convened by the department.
IU MPAS students must:
a) Use the IU EXCHANGE email address assigned upon matriculation to the program.
b) Check their IU email account and CANVAS at least once every 24 hours, and to respond to faculty (including instructional faculty) within 24 hours.
It is prohibitive to record lecturers (including principal faculty, adjunct faculty and guest lecturers) without the expressed permission of the lecturer. Students found to violate this policy will undergo a professionalism review and may be dismissed from the program.
Cell phones and other electronic devices must be on silent mode prior to class unless otherwise approved by the Course Instructor/Course Director.
If an emergency should arise while a class is in session, friends and family may contact the IU MPAS Program (317.278.9552) or the School of Health & Human Sciences main office (317.274.7447).
Each class will elect a class representative who may bring issues that affect the entire class to the attention of the Program Director.
The Physician Assistant Student Society-Indiana University (PASS-IU) will represent the entire IU MPAS student body – all active student cohorts collectively. This organization will hold officer elections and organization meetings as needed to determine the consensus of the entire PA student body regarding any issues that may affect it. A Faculty Advisor will be assigned to the PASS-IU to aid in the use of resources and will help coordinate activities within the Student Academy of the American Academy of Physician Assistants (SAAAPA) and IU Indianapolis student organizations.
On a periodic basis the IU MPAS Program Director will meet with the PASS-IU president, vice president, treasurer, secretary, and class representative to discuss any outstanding issues and to answer any questions. For issues affecting individual students, however, students are encouraged to make individual appointments with the Program Director or the student’s faculty advisor. The Program Director will communicate relevant issues to the faculty.
Article I: Section M
STANDARD A3.02The program publishes, makes readily available, and consistently applies a policy that PA students are not required to work for the program.
STANDARD A3.03The program publishes, makes readily available, and consistently applies a policy that PA students do not substitute for or function as: a) instructional faculty, b) clinical or administrative staff
STANDARD A3.14The program publishes, consistently applies, and makes readily available to enrolled and prospective students: i) policy for student employment while enrolled in the program
Training to become a physician assistant demands a full-time commitment. Due to the rigorous nature of the curriculum, it is strongly recommended that students not engage in outside employment. If a student chooses to work during the academic year, the work schedule must not interfere with class performance or clinical rotation schedules.
At no time will a student be required to work for the IU MPAS program. Further, students must not substitute for or function as instructional faculty. Students with specific prior knowledge, experiences and skills may assist faculty in didactic and laboratory sessions to share their knowledge and skills. Students will not be the primary instructor or instructor of record for any component of the curriculum.
To maintain security during examinations, exam proctors reserve the right to inspect anything a student brings into an examination room. Students are only permitted to bring the following items into the examination area: an electronic device compatible with the exam software, a charger, a writing implement. Scratch paper will be provided by the department and will be collected at examination’s end. Students are permitted to bring white boards and must demonstrate the white board is cleared before and after the exam.
During a student’s first fifteen months in the program the student will observe the usual academic calendar with respect to holidays issued by the University since students are in class for this portion of the curriculum: https://indianapolis.iu.edu/academics/calendars/. Vacation (inter-semester breaks and spring break) will be determined by the IU MPAS program and will be distributed during orientation.
During the clinical phase of the program, a student may experience a schedule different from the IU Indianapolis Academic Calendar. Clinical students should not make travel arrangements until after consulting with the Clinical Education Director.
In the event of severe weather, students should check with the IU Indianapolis webpage or watch local new channels. Students are encouraged to sign up for campus text alerts. Students are expected to use their best judgment in deciding whether or not to travel. Students on rotation sites not affected by the adverse weather are required to attend their rotation even if the campus is closed.
Conversely, students at a clinical site experiencing significant adverse weather conditions must use their best judgment in consultation with their Clinical Preceptor to determining attendance at the site regardless of the University’s status. Students must notify the IU MPAS Program (317.278.9552) of the absence as noted in Section H: Absence of this handbook.
Article II: Policies, Procedures, & Objectives Related to Clinical Rotations
STANDARD A1.01 When more than one institution is involved in the provision of academic and/or clinical education, terms are clearly described and documented in a manner signifying agreement by the involved institutions. Signed affiliation agreement(s):
a) define the rights and responsibilities of each party related to the educational program for students
b) specify whose policies govern the student, including if certain program policies will be superseded by those at the clinical site
c) include the terms of participation for the PA program students
d) are signed by an authorized individual(s) of each participating entity
STANDARDS A3.08 The program publishes, makes readily available to current and prospective students, and consistently applies a policy stating that PA students are not required to provide or solicit clinical sites or preceptors.
Most physician assistant students eagerly look forward to beginning clinical rotations. Each clinical environment holds different challenges, different rewards and serves as the starting point in the transition from student to clinician.
Indiana University has affiliation agreements in place with clinician offices and healthcare institutions allowing for a complete course of clinical rotations to be set up for each student by the IU MPAS Program. In general, rotations are assigned based upon their availability and student fit. Students will be afforded the opportunity to select specialties of interest for elective rotations. It is also possible for a student to set up a rotation outside of the IU MPAS Program’s present list of clinical sites; however, students are not required to provide or solicit their own clinical sites.
STANDARD A2.16 The supervised clinical practice experience (SCPE) instructional faculty consist of any of the following: a) PAs who hold or have held NCCPA certification, b) physicians who hold or have held board certification, c) advanced practice nurses who hold or have held board certification, d) no more than 10% other clinicians who are vetted by the program as qualified
STANDARD B3.05 Supervised clinical practice experiences collectively support the achievement of learning outcomes across the following domains: a) medical knowledge, b) interpersonal skills, c) clinical skills, d) technical skills, e) professional behaviors, f) clinical reasoning and problem-solving abilities
STANDARD B3.03 Supervised clinical practice experiences must enable all students to meet the program’s learning outcomes for: a) preventive patient encounters, b) acute patient encounters, c) chronic patient encounters
STANDARD B3.04 Supervised clinical practice experiences occur in the following settings: a) emergency department, b) inpatient, c) outpatient, d) operating room
STANDARD B3.06 Preceptors for supervised clinical practice experiences enable students to meet program-defined learning outcomes for: a) family medicine, b) emergency medicine, including providing emergent care, c) internal medicine, including elderly patients, d) surgery, including pre-operative, intra-operative, and post-operative care, e) pediatrics, including care for infants, children, and adolescents, f) women’s health, including prenatal and gynecologic care, g) behavioral and mental health care
In the IU MPAS program, clinical rotations are assigned to students based on availability. Students will complete all required rotations by the last semester of the program to be eligible for the cohort’s program completion date.
The required core clinical rotations are:
Family Medicine
Surgery
Pediatrics
Women’s Health
Behavioral Medicine
Emergency Medicine
Internal Medicine (inpatient)
Students are required to complete four clinical year electives in a discipline of interest. Assignment to specialties may vary depending upon site availability.
Students may occasionally want to develop a new rotation site. Some students may wish to rotate through a specialty or clinical site that is not currently available to the IU MPAS Program. Others may desire to rotate close to home to establish contacts for future employment. The IU MPAS Program will attempt to accommodate these requests. Students should recognize that, when possible, it may often take months to set up such a rotation.
Students should observe the following:
a) Allow at least six months for the necessary paperwork to be completed for rotations within the United States, but no less than 90 days from the beginning of the rotation being sought.
◦ The student must identify a preceptor for the Clinical Education Director to contact to obtain the preceptor’s CV and preceptor’s credentials and to discuss the site and preceptor meet program expectations for that rotation.
◦ Following review of preceptor and site, the department will request the university initiate an affiliation agreement with the site.
◦ Requests outside this timeline may not receive approval of affiliation agreements in time to begin the rotation, and requests less than 90 days from the rotation will not be pursued. It is advised students do not make travel arrangements until notification of university approval of affiliation agreement. See International Clinical Rotations (Article II: 4. International Clinical Rotations) for pursuing international rotations.
b) Ask the Clinical Education Director to contact the physician/preceptor and make all necessary arrangements at a site you have identified.
c) A family relative may not serve as the student’s preceptor.
STANDARD A1.10 The sponsoring institution: b) ensures that clinical sites and preceptors located outside of the United States are only used for elective rotations.
The IU MPAS Program does not permit international clinical rotations due to the difficulty in ensuring that appropriate training experiences are provided, and that student safety is maintained in international settings.
All clinical rotations must be completed at sites located within the United States.
Article II: Section B
Section B: Rotation specific policies
In addition to assignments required by the IU MPAS Program, some rotation sites may have specific assignments required of students. Assignments may include, but are not limited to: papers, examinations, presentations, or attendance at lectures. Students should regard these assignments as requirements for successful completion of the rotation.
Some rotations may allow a student to record information into a patient’s medical record. Students must be aware that such entries into the chart serve as a permanent part of the patient’s legal medical record. Any time a student makes an entry into the chart, it will be signed by the student. The student will indicate their physician assistant student status by writing “PA-S” following their signature. Students must ensure that their chart entries are countersigned by their preceptor as soon as possible or as required by facility policy.
Learning to document properly is an essential medical skill. During rotations where students are not permitted to record information in patient charts, they are encouraged to practice documentation separately and have it reviewed by their Clinical Preceptor.
All patient information must be held in strict confidence. Upon admission and yearly thereafter, IU MPAS students are required to successfully complete HIPAA Training. Any breach of patient confidentiality will be regarded as a serious offense and may result in dismissal from the IU MPAS Program.
STANDARD A3.04 The program publishes, makes readily available, and consistently applies a policy that requires PA students to be clearly identified in the clinical setting to distinguish them from other health profession students and practitioners.
Students must prominently display appropriate identification including their name and Physician Assistant Student either with their program-distributed ID badge or via their embroidered white coat. In addition to an identification badge, students shall state truthfully and accurately their professional status in all transactions with patients, health professionals and other individuals for whom or to whom they are responsible. While in the IU MPAS Program, students may not use previously earned titles - i.e. RN, MD, DC, PhD and EMT. Students will sign all documentation with their full name followed by “PA-S.”
Clinical sites may require that a student present immunization records prior to or on the first day of the rotation.
Sites may also require proof of a tuberculosis screening. The IU MPAS Program requires that all students receive an annual tuberculosis skin test, though clinical sites may require a different frequency.
Some sites require an annual influenza immunization. The IU MPAS Program requires that all students receive annual immunization against influenza. The influenza vaccine is available at the Student Health Clinic located in Lockefield Village: https://studentaffairs.indianapolis.iu.edu/health/medical/index.html
As graduation approaches, it is expected that students will need time to interview for employment. Requests for time-off for interviews must be approved by the IU MPAS Clinical Education Directors first. After program approval the student must clear the request with the student’s Clinical Preceptor. Students are permitted up to two (2) days off for interviews during any one given rotation during the Spring and Summer semesters. There is no maximum allowed time off for interviews during elective rotations.
A student’s primary concern should be the health and safety of the patient. Students are expected to exercise good judgment and immediately notify their Clinical Preceptor of any circumstances which may lead to patient harm. The student shall have ongoing consultation with the supervising physician as required to safeguard and enhance the care of the patient and to ensure the development of clinical skills. Students will perform only procedures authorized by the preceptor, and all procedures should be performed under the supervision of a preceptor.
While on rotation, physician assistant students function as part of a healthcare team. As such, it is frequently necessary to put the needs of the team ahead of personal interest.
It is not only important that the student receives clinical experience but also experiences the rotation as it would be in a professional practice environment following graduation. Therefore, it is expected that students will work the schedule directed by their preceptor, including "JB" and weekends, and should average at least 36 hours per week participating in educational activities for the respective clinical rotation.
STANDARD A3.03 The program publishes, makes readily available, and consistently applies a policy that PA students do not substitute for or function as: a) instructional faculty, b) clinical or administrative staff
The student is not considered an employee of any clinical affiliate and should not be a substitute for or take on any responsibilities of regular staff. If a student has a concern about the responsibilities assigned by the clinical site, the Clinical Education Director should be contacted immediately.
Listed below are guidelines which a PA student may be permitted to do by the preceptor. Please note that these are guidelines only. The judgment of the preceptor regarding how much responsibility a student is ready to assume should be the guideline for determining which tasks are assigned and how much supervision is needed.
Typical tasks assigned to PA students may include:
a) taking histories and performing physical examinations
b) assessing common medical problems and recommending appropriate management
c) performing and assisting in diagnostic and therapeutic procedures
d) assisting the preceptor in hospital/nursing home rounds, recording progress notes, transcribing specific orders of the preceptor – as allowed by the facility
e) presenting patient cases orally and in a written problem focused note format
f) discussing the basic pathophysiologic mechanisms that have produced the signs, symptoms, and disease processes under investigation
g) completing assigned readings and preparing presentations as requested by the Clinical Preceptor and/or program faculty
h) attending all teaching rounds and conferences, and
i) following the assigned on-call schedule.
Students will deliver care to patients without regard to race/ethnicity, age, gender, creed, socioeconomic status, political persuasion, sexual preference or national origin.
Most rotation sites will have their own policies and procedures that must be followed. These policies may relate to orientation sessions, parking, identification, etc. It is expected that students follow these policies. If questions regarding these policies arise, please consult with your Clinical Preceptor or the IU MPAS Clinical Education Director.
Students are responsible for arranging travel to all clinical sites and any associated fees (i.e., parking, living expenses, housing, drug testing, background check, etc). Some sites may be reached by public transportation, but most students will require a car for reliable transportation. Students may be required to travel to distant sites outside of Central Indiana for rotations. Students will be responsible to arrange and pay for their own living/housing arrangements at distant sites.
STANDARD B3.02 The program’s process clearly documents the initial and ongoing evaluation of all sites and preceptors used for supervised clinical practice experiences, to ensure students have access to: a) the physical facilities needed to meet the learning outcomes for the specific SCPE, b) patient populations needed to meet the learning outcomes of the specific SCPE, c) supervision
A faculty member performs on-site visits. The purpose of the site visit is two-fold. First, as per the ARC-PA standards, clinical sites must be assessed continually to make sure the site is student ready and is an appropriate and quality teaching environment.
During a site visit, a faculty member will meet with students and discuss the rotation.
Site visits for all rotations may be arranged randomly at the discretion of the IU MPAS Program. Site visits may occur during any rotation and may be unannounced. A site visit evaluation form or an online equivalent (via eMedley) will be completed by faculty after each site visit.
Article II: Section C
The IU MPAS program uses an internet-based system to assist with collecting documentation. The system is called eMedley. Orientation regarding the operation of this system will be provided to students prior to beginning clinical rotations.
STANDARD A3.14 The program publishes, consistently applies, and makes readily available to enrolled and prospective students: a) any required academic standards to maintain enrollment and progress in the curriculum, b) requirements and deadlines for completion of the program, c) policies and procedures for remediation, d) policies and procedures for deceleration, e) policies and procedures for withdrawal, f) policies and procedures for dismissal
STANDARD B3.05 Supervised clinical practice experiences collectively support the achievement of learning outcomes across the following domains: a) medical knowledge, b) interpersonal skills, c) clinical skills, d) technical skills, e) professional behaviors, f) clinical reasoning and problem-solving abilities
STANDARD B3.03 Supervised clinical practice experiences must enable all students to meet the program’s learning outcomes for: a) preventive patient encounters, b) acute patient encounters, c) chronic patient encounters
STANDARD B3.04 Supervised clinical practice experiences occur in the following settings: a) emergency department, b) inpatient, c) outpatient, d) operating room
STANDARD B3.06 Preceptors for supervised clinical practice experiences enable students to meet program-defined learning outcomes for: a) family medicine, b) emergency medicine, including providing emergent care, c) internal medicine, including elderly patients, d) surgery, including pre-operative, intra-operative, and post-operative care, e) pediatrics, including care for infants, children, and adolescents, f) women’s health, including prenatal and gynecologic care, g) behavioral and mental health care
Clinical rotations are graded on a Satisfactory/Fail grading scale.
Satisfactory: Signifies satisfactory performance
Fail: Signifies the student has not performed satisfactorily
Clinical logs in eMedley are designed to help the program track a student’s experiences through clinical rotations. Completing logs thoroughly and accurately IS MANDATORY and will help ongoing program evaluation and accreditation purposes. Logs must be kept up to date and students are expected to input data on a daily basis, including documenting duty hours each day. Failure to not log any patient encounters during any given rotation by the last day of that respective rotation will result in a deceleration and delay in the progression of the clinical year. Documentation of patient demographics, diagnoses seen and procedures performed will be submitted through the eMedley system. Frequently employers ask the PA program to provide information regarding the number and types of patients a student has seen. They also ask for a list of procedures performed by a student. Only the information reflected in the eMedley logs will be shared with student permission via the student file release form. Thus, it is in the student’s best interest to accurately and thoroughly complete these logs. Completing these logs leads to successful completion of the rotation.
Any falsification of clinical logs or duty hours will result in a professional review for recommendation of a disciplinary action.
a. Assignments will be required for each rotation.
b. Assignments must be turned in on time and meet the passing criteria.
c. Failure to turn in assignments will result in a course failure.
d. Unsatisfactory completion of assignments may result in course failure.
The IU MPAS faculty developed a competency list which are considered essential skills for practicing as a physician assistant. Each competency listed is required to be signed off by your preceptors throughout the clinical year indicating you have gained mastery of the skill. At the beginning of each rotation, you will discuss which competencies you are required to complete within a specific rotation (i.e. writing a discharge summary during your internal medicine rotation, performing an incision closure during your surgery rotation) and which other competencies you desire to complete. When you feel you are competent in a specific skill you will request your preceptor to observe you completing these skills and have them sign off that you were competent in that skill. If your preceptor does not think you are competent then you will be requested to complete the skill until you have gained mastery. All skills on this list must be deemed competent to graduate. To graduate, you must have your entire list signed off by the end of the second week of your last core rotation. You will not be able to meet these competencies via cases with faculty.
Each core rotation (non-specialty selective and elective) will have a small subset of competencies that must be completed during that rotation. These competencies are expectations consistent with the course syllabi for that rotation. These items are demarcated with the abbreviation of the course in red. The key to the course abbreviations will follow this page. The remaining competencies may be completed at any point during your clinical year. The list is separated into general skills, pediatric-, ob/gyn-, surgery-, emergency medicine- and behavioral medicine-specific.
Your check offs will be reviewed via an assignment on Canvas during your rotation and again at the end of the core rotations prior to electives.
The full list of clinical year competencies can be found in the cohort’s Canvas site prior to the beginning of the clinical year.
The following list is the program expectation for minimum patient encounters to be achieved during the clinical year. These encounters must be documented in eMedley. The clinical education director and the chair of the program/evaluation committee will review the student logs every three rotations to track student progress to completing these minimum requirements. If a student is unable to meet the minimum encounters prior to the start of rotation 11, the student will be placed in a clinical setting(s) during the last rotation to fulfill the outstanding requirement(s).
| Minimum Patient Encounter Requirements | |
| Encounter Type | Minimum Number of Documented Encounters |
| Infant (<1) | 5 |
| Child (1-12) | 24 |
| Adolescent (13-17) | 8 |
| Adult (18-64) | 148 |
| Elderly/Geriatric (65 and older) | 39 |
| Acute | 122 |
| Chronic | 142 |
| Emergent | 10 |
| Preventive | 124 |
| Prenatal | 5 |
| Gynecologic | 11 |
| Behavioral/Mental Health | 15 |
| Pre-operative | 8 |
| Intra-operative | 3 |
| Post-operative | 17 |
Mid-rotation feedback is designed to give students an opportunity to request feedback on their performance during each clinical rotation. It is the student’s responsibility to initiate the performance feedback with their preceptor(s) utilizing the mid-rotation evaluation form for guiding feedback questions.
The mid-rotation self-assessment is designed for the student to self-reflect on clinical experiences and to identify areas of improvement as well as strengths. Students should take this information as an opportunity to strengthen skills to meet course learning outcomes assessed at the end of the rotation. If any academic or clinically related problems arise from this evaluation, it is in the student’s best interest to discuss the issue with the course director. The student is expected to complete the self-assessment by end of day on the third Monday of the rotation. It is expected that all questions on the assessment are complete. Course directors will review the self-assessment and provide feedback if appropriate in the respective Canvas course.
The program has adopted a standard rubric for clinical preceptors to use to evaluate student competency. Evaluations should be completed by preceptors online through the eMedley system. Sometimes preceptors will request paper copies of the evaluation, which will be transcribed into eMedley by clinical year staff. Preceptor evaluations are based on direct observations of student performance. This evaluation is a formative assessment, and the feedback is intended to facilitate student proficiency in their clinical reasoning, communication, professionalism, and skills necessary for entry level practicing PAs. An evaluation that is deemed “satisfactory” for the rotation is determined by the ability of the student to demonstrate learning outcomes and competencies essential for clinical practice a new graduate.
In some instances, particularly in emergency medicine and family medicine, a resident or another attending physician may complete a preceptor evaluation form in addition to the Clinical Preceptor of record. Although it is thoroughly indicated that it is the responsibility of the preceptor of record to complete an evaluation for the students precepted, it is the IU MPAS program's policy that after 2 failed attempts to contact the preceptor of record about filling out an evaluation, the student will receive a passing grade without feedback.
All evaluations for a respective course will be taken into consideration in determining the final course grade.
Students will complete two end-of-rotation evaluation forms: 1) preceptor and clinical site and 2) rotation course. The student evaluation is designed to provide the IU MPAS Program with student feedback regarding each clinical site and preceptor. The Program uses this feedback to evaluate and improve the clinical site and preceptor teaching which, in turn, improves a student’s clinical experience. This process is important for continued quality control and accreditation. Evaluations of clinical sites and preceptors will be completed online using the eMedley system.
This clinical rotation course evaluation is to evaluate the administrative aspects of the clinical rotation course such as assignments, syllabus, communication with the course director of the respective rotation. Evaluation of courses is an accreditation requirement and fosters the department’s ongoing program evaluation.
An End of Rotation (EOR) examination is given after the following core rotations: women’s health, surgery, internal medicine inpatient, family practice, community medicine, emergency medicine, behavioral health and pediatrics rotation and is based on course learning outcomes and instructional objectives for that rotation. Refer to course syllabi for rotation specific objectives. The blueprints and topic list for the exams can be found: https://paeaonline.org/assessment/end-of-rotation/content
The majority of EOR exams are given the Friday of the last week of the scheduled rotation. The exams should be administered on campus and proctored by trained staff. Students should check their university exchange email accounts for any special instructions regarding EOR exams. Students must bring their university ID.
PAEA EOR exams are graded on an objective basis using multiple choice questions.
For each exam there are 2 or 3 forms, which are designated to each student by PAEA. There are no PAEA examinations specifically written for community medicine clinical rotations, though community medicine encompasses primary care across the lifespan. The family medicine EOR examination developed by PAEA has three forms, thus the family medicine EOR will also be used for the community medicine rotations.
PAEA EOR exam scores will be normalized against national data. There are published national scale score means and standard deviations for each form. A student must achieve a passing grade, which is defined by the program (Z-score > -1.50), with the normalized score [Z= (Student Scale Score-National Scale Mean)/Standard Deviation].
Students who receive a grade equal to or below a Z-score of -1.50 on an EOR exam will have a second opportunity to pass the EOR exam within 1 month of the release date of the EOR exam grade. The program will determine the date and time. Should the student fail one of the forms of the family medicine examination, another form of the exam will be utilized, though the program will have to invalidate a prior exam through the PAEA portal since the student may only have three versions completed at any given time. Should this no longer be an option, the student will take a program developed exam for the retake. The PAEA assessment package, which includes PACKRAT, EOR exams and the End-of-Curriculum exam permits for up to two repeat examinations without extra cost to the student. If more than two repeat exams are required, the student is responsible for the expense of the repeated EOR exam and must provide payment to the Program no later than three days prior to the scheduled retake If the student fails the second attempt, the student will enter the remediation process as outlined in this manual. Failure to pay for or take the repeated exam at the designated time/date will result in an automatic course failure. See Clinical Remediation Policy.
In certain situations (including but not limited to having a previous course failure), a student may be granted one opportunity to interrupt their clinical year to take a four-week remediation period after failure of an initial end-of-rotation exam. The student will meet with a principal faculty member to develop a remediation plan and contract for the four weeks. At the conclusion of the four-week remediation period the student will be expected to take the second iteration of the end-of-rotation examination. If the student passes the retake examination, they will resume their clinical rotations with their rotation group. It will be necessary for the student to decelerate their program completion and make up the missed rotation during the remediation period following completion of all core rotations. Availability of clinical rotation sites will determine the student’s new program completion date. If the outcome is failure of the retake examination, appropriate remediation or dismissal policy will go into effect. This clinical remediation period does NOT count towards the only one course remediation permitted policy.
Students are permitted to take end-of-rotation examinations that occur between consecutive out-of-state rotations at an approved testing center, provided they arrange and bear the associated costs. For other circumstances, approval will be made on a case-by-case basis by the Program Director or Clinical Education Director.
Students will return to campus for four immersion weeks during the clinical year. Students must attend all Immersion Week lectures and activities. Students will be notified in advance of any schedule changes, but students should be available 8am-5pm on these days.
Immersion Week instructional and assessment activities are outlined in each of the respect course syllabi – See individual course learning outcomes and instructional objectives. Examples include but are not limited to the following:
• Assessment of program and clinical year competencies
• Case-based learning activities
• Lectures, including employment and professional seminars
• Student presentations
• Reflection assignments
• PANCE review
• Advising meetings with Faculty Advisors and Course Directors
• Meetings to complete required paperwork with Faculty Advisors and Course Directors
The criterion for a failing grade for a rotation is any one of the following:
• Failure of initial and repeated EOR exam.
• Failure to demonstrate proficiency in the course learning outcomes
• Failure to timely submit required course assignment(s) and earn passing grade on each
• Failure to demonstrate competency on preceptor evaluation, which includes professionalism.
STANDARD A3.14 The program publishes, consistently applies, and makes readily available to enrolled and prospective students: c) policies and procedures for remediation, d) policies and procedures for deceleration, e) policies and procedures for withdrawal, f) policies and procedures for dismissal
If a student does not demonstrate proficiency in course learning outcomes based on clinical preceptor evaluation, is given a course failure due to unprofessionalism conduct, failure of course required assignments, or receives a course failure for two failed end of rotation (EOR) examinations in the same rotation the student will enter remediation by repeating the entire clinical rotation course, including exams and assignments where applicable. The remediation process is defined in each syllabus. The course director will report the course grade to the registrar as “F” and the student will register for the course again during summer session II, though will not complete the rotation until the conclusion of all other rotations, which may require earning an “incomplete” during summer session II until all components are completed satisfactorily. The student will receive “Satisfactory” for the course following successful remediation. If a student does not successfully remediate, the course director will report an “F” to the registrar on the repeated course and the student will be dismissed per the two-course failure policy. The student’s file will reflect the initial failing grade and remediation.
This repeated clinical rotation may only occur at the end of all other core rotations, which will result in a delay of graduation. Depending on the clinical rotation, the student will complete either an IUMPAS faculty-created examination or a PAEA examination at the end of this repeated rotation. If the student has not already used all the EOR examinations in the PAEA Assessment Package, the student is responsible for the expense of the repeated PAEA EOR exam(s) and must provide payment to the Program no later than three days prior to the scheduled retake. The deferral of the remediation to end of the clinical year ensures the student will have available PAEA exam(s) for the end-of-rotation exam since PAEA releases new versions in July.
The remediated course will follow the same minimum grade requirements as described in End of Rotation Exam (EOR) Examinations (see 8. End of rotation (EOR) examinations) and the process for repeated exam during that rotation. The student has the opportunity to remediate the exam content with the course director during the repeated rotation. Each student has access to their PAEA EOR exam breakdown to utilize as a study aid during the remediation process. The scheduled remediation meetings are at the discretion of the course director.
Article II: Section D
Section D: Tips for successful clinical rotations
a) Know the Clinical Site:
1) You should review your information sheet for your next rotation as soon as you receive it to find out about credentialing, parking, ID’s, orientation, etc.
2) Every effort has been made to maintain and update appropriate contact information for clinical sites. Nevertheless, minor problems may occur. It is necessary to maintain professionalism and flexibility when faced with such changes. First, try to resolve any discrepancies on your own. Call the Clinical Education Director if this is not possible. Notify the Clinical Education Program Assistant of any errors in supplied instructions so corrections may be made.
3) Find out what available conferences/lectures you might attend (grand rounds, daily/weekly conferences, CME presentations, etc.)
4) Be sure to secure housing before you arrive to the clinical site. Students are expected to arrange and pay for their own living arrangements.
b) Important Items to Discuss with Your Preceptor:
1) Confirm your time schedule and specific duties - when to report to your rotation, on-call schedule, rounds, weekend hours, etc.
2) Determine which competency skills must be completed for the rotation and articulate to your preceptor.
3) Identify special interests you have, whether it is procedures you would like to experience or particular cases you would like to see relevant to the rotation.
4) Talk to preceptors about technical procedures and your eagerness to participate in performing them.
5) Ask what is expected of you.
c) Additional Considerations:
1) What you gain from the rotation is equal to the effort you put forth.
2) Be courteous to everyone.
3) Develop and maintain a professional attitude.
4) Be helpful to the preceptor and staff.
5) Take initiative.
6) You may encounter harsh criticism at times. Try to learn from the feedback.
7) Be prepared to discuss and answer questions about any disease or procedure encountered during your rotation.
8) Read about the disease processes you encounter each day.
9) Be prepared to study and read at least two hours per day outside the clinical rotation hours.
10) You may not always be permitted to write on charts. If this is the case at your site, practice writing notes on a separate sheet and have preceptors critique them.
11) While on rotations, actively look for work.
12) Report early, stay late, volunteer for call.
13) Maintain strict confidentiality at all times.
14) Follow guidelines regarding social media use.
15) Have a positive attitude.
If any concerns arise during rotations, please notify the Clinical Education Director or your Course Director as soon as possible. If unable to contact the Clinical Education Director or Course Director, please contact your faculty advisor or the program director.
The table below summarizes requirements associated with clinical rotations.
| Requirements | Responsibility | Format | Due |
| Review of Goals & Objectives & Competencies | Student & Preceptor | eMedley | First week of each rotation |
| Competency List | Student & Preceptor | Paper | Last day of each rotation |
| Minimum patient encounters | Student | eMedley | End of clinical year |
| Mid-rotation Self-Assessment and Preceptor Feedback | Student & Preceptor | Online/eMedley | 3rd Monday of each rotation |
| Mid-rotation communication with faculty | Student & Faculty | Midpoint of each rotation after student completes their self-assessment and preceptor feedback | |
| Preceptor Evaluation | Preceptor | Online/eMedley | Last day of each rotation |
| Student Evaluation of Clinical Site | Student | Online/eMedley | Last day of each rotation |
| Written Materials | Student | Online submission | Last day of each rotation |
| Connect with student previously at the next assigned site/preceptor | Student | Verbal or Email | Last week of each rotation |
| End of Rotation Examination (if applicable) | Student | Online | Last day of each rotation |
Article III: Preparing for graduation & the Physician Assistant National Certifying Exam (PANCE)
STANDARD B4.03 The program conducts and documents a summative evaluation of each student within the final four months of the program to verify that each student meets all program-defined competencies required to enter clinical practice, including: a) clinical and technical skills, b) clinical reasoning and problem-solving abilities, c) interpersonal skills, d) medical knowledge, e) professional behaviors
STANDARD A3.14 The program publishes, consistently applies, and makes readily available to enrolled and prospective students: a) any required academic standards to maintain enrollment and progress in the curriculum, b) requirements and deadlines for completion of the program, c) policies and procedures for remediation, d) policies and procedures for deceleration, e) policies and procedures for withdrawal, f) policies and procedures for dismissal
Summative Evaluations occur within the student’s last four months of the program and following completion of all core rotations.
This exam tests a student’s knowledge base on all organ systems. Any student who fails to achieve a passing grade will earn an incomplete in the MPAS M700 Graduate Preparedness for Entry Level Practice and enter remediation.
• Due to this the student will have a decelerated program completion date.
• Once the student has demonstrated competency during remediation SPC will determine the date of the reassessment and revised program completion date. The minimum interval between exams is determined by SPC and is guided by the exam developer.
This hands-on examination is designed specifically to test the PA student’s clinical competence. Students must demonstrate competency in all components of the multi-part practical skills assessment. Any student who fails to achieve a level 3 (competent) in each IU MPAS competency domain will earn an incomplete in the MPAS M700 Graduate Preparedness for Entry Level Practice and enter remediation.
• Due to this the student will have a decelerated program completion date.
• Once the student has demonstrated competency during remediation SPC will determine the date of the reassessment and revised program completion date. The minimum interval between exams is determined by SPC.
Article III: Section B
Section B: Program exit surveys and interview
An exit survey and competency survey will be disseminated electronically during the final month of the student’s respective program completion date. Group exit interviews will be conducted during the last week of the cohort’s program; students with decelerated program completion dates will participate in the group interviews with their matriculated cohort. These items are components of the requirements for graduation from IU MPAS.
No student will be eligible for program completion until the student has completed all program requirements. |
Article III: Section C
The clinical phase of training comes at the end of the IU MPAS Program, as does studying for the Physician Assistant National Certifying Examination (PANCE). It is difficult to study for the PANCE during rotations because parallel processes are occurring: a student is acquiring new clinical skills and studying specific topics for the end of the rotation examination, while trying to broadly prepare for the PANCE by studying many other diseases perhaps unrelated to the current rotation. For this reason, the processes have been integrated to minimize duplication of study and create synergy. As a result, if a student studies all the topics listed for each rotation, by the time that student finishes rotations, he/she will have studied all of the topics included in the National Commission on Certification of Physician Assistants (NCCPA) Content Blueprint for PANCE & PANRE (Physician Assistant National Recertifying Examination).
Many questions on the PANCE are drawn from the 2019 NCCPA Content Blueprint. The Content Blueprint comprises two helpful documents: the “Content Blueprint Sample Disease/Disorders by Organ System” and the “Content Blueprint Physician Assistant Practice Task Areas.” Both students and faculty use these documents to know which topics are important and the depth and breadth at which they should be covered (https://www.nccpa.net/pance-content-blueprint).
The organ-system blueprint is a comprehensive list of diseases and disorders commonly encountered in clinical practice and thus on the certification examinations. The list (see TABLE 1: PANCE MEDICAL CONTENT CATEGORIES below) is arranged by organ system and also indicates the approximate percentage of questions per organ system you may expect on the PANCE. This information is important to consider when deciding the depth and breadth of study. Because cardiovascular, pulmonary, gastrointestinal/nutritional and musculoskeletal topics comprise a large portion of the exam (about 40% of the exam questions), faculty and students spend more time on them. Students who have a poor knowledge base in these four organ systems generally receive poor grades on the PANCE.
The task-areas blueprint is a list of seven main PA knowledge areas that have been identified as important to clinical practice. It details the cognitive skills and knowledge in each area that students must attain for competence. Many of these task areas are covered on the PANCE. Since it is impossible to study everything about every item in the Content Blueprint, this document helps you determine what is most important to know.
The task-areas blueprint also indicates the approximate percentage of questions per task you may expect on the PANCE and PANRE. This is helpful as you begin studying, so that you may focus your efforts on task areas more commonly seen on the exams. The organ systems and task areas more heavily weighted by the NCCPA receive more in-depth treatment on the NCCPA exam.
The formulation of a comprehensive and effective study plan requires consideration of many factors. Haphazard, non-strategic studying that does not take into account the NCCPA Content Blueprint, the weighting of task areas and organ systems, and your own strengths and weaknesses can lead to disaster. In addition to testing specific blueprint topics there will also be some case-based questions that are not specifically linked to a blueprint topic but are discipline related and will test knowledge and skills gained at the rotation site.
PA students typically are overwhelmed by the amount of time they must spend at the clinical site during a rotation, and how little time is left for actual study. Therefore, it is important to set short-term (daily), intermediate (weekly) and long-term (end-of-rotation) study goals. For example, a student should calculate how many topics must be covered daily to be ready. The student must take charge of their own learning by determining how to manage a personal schedule in order to be able to complete and study the required topics within the timeframe that has been set. Students should also dedicate a few extra days before any testing cycle for review and reinforcement of materials learned. Because each student knows their own learning style best, taking the time to thoughtfully set a study schedule is critical.
PANCE Content Blueprint (effective for all PANCE administrations beginning in January 2025)
TABLE 1: PANCE MEDICAL CONTENT CATEGORIES
| Medical Content Categories | Percent Allocation* |
| Cardiovascular System | 11% |
| Dermatologic System | 4% |
| Endocrine System | 6% |
| Eyes, Ears, Nose, and Throat | 6% |
| Gastrointestinal System/Nutrition | 8% |
| Genitourinary System (Male and Female) | 4% |
| Hematologic System | 5% |
| Infectious Diseases | 7% |
| Musculoskeletal System | 8% |
| Neurologic System | 7% |
| Psychiatry/Behavioral Science | 7% |
| Pulmonary System | 9% |
| Renal System | 5% |
| Reproductive System (Male and Female) | 7% |
| Professional Practice | 6% |
2. TABLE 2: PANCE EXAM CONTENT BY TASK AREA
| Task Categories | Percent Allocation* |
| History Taking and Performing Physical Examination | 16% |
| Using Diagnostic and Laboratory Studies | 10% |
| Formulating Most Likely Diagnosis | 18% |
| Managing Patients | |
| Health Maintenance, Patient Education, and Preventive Measures | 11% |
| Clinical Intervention | 16% |
Pharmaceutical Therapeutics | 15% |
| Applying Basic Scientific Concepts | 8% |
| Professional Practice | 6% |
Tables 1 and 2 Adapted from the National Commission on Certification of Physician Assistants: NCCPA-Connect. https://www.nccpa.net/pance-content-blueprint
Article IV: Appendices
Accreditation Review Commission on Education for The Physician Assistant, Inc. (ARC-PA) |
The Accreditation Review Commission on Education for the Physician Assistant (ARC-PA) is the recognized accrediting agency that protects the interests of the public and PA profession by defining the standards for PA education and evaluating PA educational programs within the territorial United States to ensure their compliance with those standards.
The ARC-PA encourages excellence in PA education through its accreditation process, by establishing and maintaining minimum standards of quality for educational programs. It awards accreditation to programs through a peer review process that includes documentation and periodic site visit evaluation to substantiate compliance with the Accreditation Standards for Physician Assistant Education. The accreditation process is designed to encourage sound educational experimentation and innovation and to stimulate continuous self-study and improvement.
American Academy of Physician Associates (AAPA) |
The AAPA is the national professional organization of physician assistants/associates. Its membership includes graduate and student physician assistants as well as affiliate membership for physicians and physician assistant educators. All Indiana University Physician Assistant Students will be Student Members of the AAPA. The Academy provides a wide range of services for its members from representation before federal and state governments and health related organizations, public education, pamphlets and brochures, insurance and financial programs, and assistance.
As an AAPA member, you also receive multiple publications and are entitled to a membership discount for the annual spring conference. Student Physician Assistant Societies are an integral part of the AAPA and make up a body referred to as the Student Academy of the American Academy of Physician Associates (SAAAPA). The Student Academy meets yearly at the national spring conference to elect Directors and representatives. Release time to attend the national conference held in May of each year can be requested from the Program and will be allowed on a case-by-case basis.
Indiana Academy of Physician Assistants (IAPA) |
The Indiana Academy of Physician Assistants (IAPA) is the officially recognized state chapter of the AAPA. IAPA was founded in 1974. Their vision is the same now as it was then—"IAPA shall be the
definitive and authoritative representative for the physician assistant profession in Indiana. It shall foster enhanced practice environments for physician assistants and support on-going professional development and intellectual enrichment. IAPA shall promote quality healthcare that is cost-effective and accessible in the state of Indiana. IAPA strives to be a representative of all physician assistants within the State of Indiana."
IAPA is an officially recognized state chapter of the American Academy of Physician Assistants (AAPA). All Indiana University Physician Assistant Students will be Student Members of the IAPA.
Physician Assistants Education Association (PAEA) |
PAEA is the only national organization representing physician assistant education programs in the United States. Currently, all of the accredited programs in the country are members of the Association. PAEA provides services for faculty at its member programs, as well as applicants, students, and other stakeholders.
The Association was founded in 1972 as the Association of Physician Assistant Programs. Member programs voted to adopt the current name in 2005.
National Commission on Certification of Physician Assistants (NCCPA) |
All graduates of Physician Assistant Programs accredited by the Accreditation Review Commission on Education for the Physician Assistant (ARC-PA) are eligible to sit for the national certifying exam (PANCE) offered by the NCCPA. Registration applications are completed during the final year of the Physician Assistant Program.
Once certified through the NCCPA, each graduate must obtain and report 100 hours of CME every two years. Currently recertification exams are required every six years in addition to the CME requirement. Beginning in 2014, certified physician assistants will transition to a 10-year certification maintenance cycle.
State agencies |
In Indiana, physician assistants are licensed under the authority of the Professional Licensing Agency (PLA). The Physician Assistant Advisory Committee reports to the PLA Board and assists in forming policy. The Program will assist students seeking licensure in Indiana with completing the application as graduation approaches. Students pursuing licensure from other states should contact that state’s licensing board or PA society for more information.
https://www.in.gov/pla/professions/physician-assistant-home/ (they changed the website so the original link doesn't work)
| Faculty/Staff Name | |
| Peter Altenburger, Ph.D., PT Associate Professor Associate Dean of Faculty Affairs | paltenbu@iu.edu |
| Jennifer Piatt, Ph.D., MS Associate Professor Department Chair | Jenpiatt@iu.edu |
| Jill Murphy, M.D. Clinical Assistant Professor Medical Director | jamenego@iu.edu |
| Lauren Gilliam, MPAS, CHA/PA-C Clinical Assistant Professor Program Director | gillilau@iu.edu |
| Ron Contreras, MSPAS, PA-C Clinical Assistant Professor | rvcontre@iu.edu |
| Kelly Fisher, MPAS, PA-C Clinical Assistant Professor Didactic Education Director | fisherkk@iu.edu |
| Nathan Rothchild, DMSc, MPAS, PA-C Clinical Assistant Professor Clinical Education Director | nlechien@iu.edu |
| Gary Long, Ph.D. Assistant Professor | garlong@iu.edu |
| Eryn Morrow, MS-PAS, PA-C Clinical Assistant Professor | erynmorr@iu.edu |
| Will Parmenter, MPAS, PA-C Clinical Assistant Professor | wparment@iu.edu |
| Elisa Sterner, MPAS, PA-C Clinical Assistant Professor | esterner@iu.edu |
| Milagros Cardona Clinical Education Program Assistant | miacardo@iu.edu |
| Peggy Wortham Administrative Coordinator | psavage@iu.edu |
Advisors will meet with their assigned advisees on a regular schedule and as needed per student request or for cause due to Student Progress Committee or Program Director request. Each encounter should be documented to address concerns and the plan, which may include follow-up meetings. Documentation will be done via Qualtrics and/or Canvas and will be stored in the student file. The Didactic/Clinical Advising Survey, located in Canvas, is to be completed prior to individual or group meetings. It will be reviewed by the faculty advisor. After the individual or group meeting, the student may add comments in the "Comments" section on the respective assignment in Canvas to summarize an overview of their meeting.
| Timeline | Scheduling Timeframe | Rationale for Meeting | Documentation |
| Week of orientation | Administrative Coordinator to arrange | Advising group meeting with all newly admitted advisees to discuss any questions regarding the department policies, to get to know the students, and to inform them of student services. | Student will complete the Advisee Information Sheet at least one day prior to the meeting The Welcome Agenda to be utilized as framework for conversations |
| Mid Semester 1 | 15–20 minute individual meetings scheduled within 1–2 weeks after first Anatomy exam. Scheduling per advisor. | Individual one-on-one advisee meetings to get to know the individual and to discuss any concerns that were mentioned in the Advisee Information Sheet | Student to complete advising survey |
| Semester 2 | On academic calendar Goal: October | Group meeting to check in | Student to complete advising survey |
| Semester 3 | On academic calendar Goal: February | Group meeting to check in | Student to complete advising survey |
| Semester 4 | Individual meetings scheduled per advisor. Goal: July/August | Review Professionalism Self-Assessment Didactic Year Tool and Advisor Professionalism Assessment. Discuss upcoming rotations, review PACKRAT report when available | June: Professionalism Assessment Didactic Year forms completed by student and advisor. July: Individually review performance report from ExamSoft & PACKRAT to navigate conversation for clinical year preparedness and promotion to the clinical year Student to complete advising survey |
| Semesters 5 and 6 | Submission of Clinical Year Advising Survey required during immersion week. Individual meetings are optional. | Review Advising Survey and provide appropriate assistance | Consider: discussion of rotations, EOR exams, budget & planning for review course (if applicable), career planning, CV review, consider advisee write own recommendation letter as a starting point |
| Semester 7 | Individual meeting following submissions for Grad Prep. Scheduling per advisor. | To review the Professionalism Self-Assessment Clinical Year Tool | Professionalism Assessment Clinical Year forms completed by student and advisor. Students to complete advising survey |
| Per student request | Student-initiated | Post-meeting documentation via Canvas | |
| Per Student Progress Committee request | SPC or course/module instructor will notify the advisor of the first assessment | ||
| Per Program Director | Program Director will notify advisor of professionalism concerns, which may results in a Professionalism Review | Program Director will document formal notification & recommended actions if there is a professionalism review committee formed Program Director will document in an email to advisor and student for concerns not going through a professionalism review and will create and Incident Report on Qualtrics |
Advisor/Advisee role regarding didactic assessment and course failures
- After an assessment or exam failure, the faculty advisor will be notified by the block director/course instructor/director of didactic education of the assessment failure/poor performance.
- After the first assessment failure throughout the didactic curriculum, the student must reach out to faculty advisor to meet and discuss ways to enhance study skills.
- https://blc.indianapolis.iu.edu/resources/index.html
- CAPS quick info sheet (in advisor folder on shared drive) online assessment tools: https://studentaffairs.indianapolis.iu.edu/health/counseling-psychological/self-screening-tools.html
- For courses requiring assessment remediation, the student must meet with the block director to review remediation procedures.
- If the advisee continues to have further poor performances throughout their didactic courses, the communication may be conducted via email if the student determines they do not need further in-person meeting with their advisor or further meetings would be perceived as burdensome to the student.
- For a course failure, the student must meet with their advisor.
Student advisee information sheet
| Name: | |
| Preferred Name: | |
| DOB: | |
| Preferred Phone #: | |
| Current Address: | |
| Faculty Advisor: |
| Relationship status: | |
| Number of Children: | |
| Are you new to Indianapolis? | ☐ Yes ☐ No |
| Do you need recommendation for a Primary Care Provider? | ☐ Yes ______________ ☐ No ______________ |
| Do you need recommendation for a dentist? | ☐ Yes ______________ ☐ No ______________ |
| Adaptive Education Services | |
| Have you reported or do you plan to report any academic or medical disabilities to Adaptive Education Services? | ☐ Yes; Please explain if you feel comfortable: ____________________________________________________ ☐ No ☐ I am not sure |
| What concerns do you have about getting through this program? |
|
| What do you like to do for fun? (Check all that apply) |
☐ Read ☐ Play sports ☐ Other ________________ ☐ Physical Activity ☐ Watch sports ☐ Play an instrument ☐ Video gaming ☐ Arts & Crafts ☐ Cooking |
If you had unlimited resources and could go anywhere in the world, where would you go and why? |
|
| What else would you like to share with me? |
|
| Didactic Course & Module Evaluation Questions |
Select your level of agreement with each of the statements using the following Likert-scale
|
| Overall, I would rate the quality of instruction as excellent. |
| The instructor was well prepared for class. |
| The instructor facilitated my ability to critically think about the subject. |
| The instructor explained concepts clearly. |
| The instructor encouraged student questions and participation. |
| The instructor presented content in an organized manner. |
| I was able to effectively communicate with my instructor. |
| The instructor is enthusiastic about teaching the course. |
| Overall, I would rate the quality of this course as excellent. |
| Announced course objectives agree with what is taught. |
| Expectations for student learning were clearly defined. |
| I learned many things I consider valuable. |
| The course developed my abilities and skills in this field. |
| The course activities, assignments, and assessments (quizzes, tests, exams) helped me learn the material. |
| Open-Ended Questions: |
| What aspects of the course do you feel were most valuable for your learning and future career? |
| What can the instructor do to improve the course or their teaching effectiveness? |
Faculty Advisor Name: __________________________________________
| 5 | Consistently exceeds expectations; outstanding performance |
| 4 | Occasionally exceeds expectations; above average performance |
| 3 | Meets expectations; average performance |
| 2 | Occasionally meets expectations; below average performance |
| 1 | Does not meet expectations; poor performance |
| N/A | Not applicable |
| Assessment Category | ||||||
| General | ||||||
| Student exhibits a positive and professional attitude. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student exhibits emotional stability, maturity, empathy and physical and mental capacity. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student maintains current immunizations, CPR, and background checks. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student acts appropriately in stressful situations. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student reports physical handicap or health issues that may interfere with their ability to perform the program technical standards or place the patient/classmate at risk. | 5 | 4 | 3 | 2 | 1 | N/A |
| Assessment Category | ||||||
| Professional | ||||||
| Student demonstrates respect for other students and faculty members. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student upholds the dress code on campus and/or clinical sites. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student is prompt and on time for classes and all activities associated with clinical rotations. Demonstrates minimal class disruption and maximum commitment and respect to the lecturer by minimizing missed class sessions, late arrivals or early departures. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student refrains from unprofessional behaviors such as talking repetitively in class during lectures/labs/grand rounds etc. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student is able to work cooperatively, preserving relationships with peers and other members of the health care team. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates full understanding of HIPAA standards, including utilization of all media devices that place patients/providers at risk. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student refrains from personal cell phone usage during rotations or class, except to utilize program/facility approved medical apps for the sole purposes of accessing info for pt. care | 5 | 4 | 3 | 2 | 1 | N/A |
| Academic | ||||||
| Student demonstrates the ability to learn and function in a wide variety of didactic and clinical settings. This includes demonstration of ongoing learning by referencing didactic content and utilizing rotation unique study references, to keep pace with evolving standard of care practices. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates effective oral, electronic and written communication, addressing individuals utilizing appropriate tone and etiquette as well as grammar. (ex. using Dr. Miss, Mrs. Etc.) | 5 | 4 | 3 | 2 | 1 | N/A |
| Student exhibits academic integrity. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates adaptability. | 5 | 4 | 3 | 2 | 1 | N/A |
| Comments |
|
Faculty Advisor Signature: _______________________ Date: _________
Student Signature: ________________________ Date: _________
Professionalism Self-Assessment Tool – Clinical Year
Faculty Advisor Name: __________________________________________
| 5 | Consistently exceeds expectations; outstanding performance |
| 4 | Occasionally exceeds expectations; above average performance |
| 3 | Meets expectations; average performance |
| 2 | Occasionally meets expectations; below average performance |
| 1 | Does not meet expectations; poor performance |
| N/A | Not applicable |
| Assessment Category | ||||||
| General | ||||||
| Student exhibits a positive and professional attitude. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student exhibits emotional stability, maturity, empathy and physical and mental capacity. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student maintains current immunizations, CPR, and background checks. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student acts appropriately in stressful situations. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student reports physical handicap or health issues that may interfere with their ability to perform the program technical standards or place the patient at risk. | 5 | 4 | 3 | 2 | 1 | N/A |
| Assessment Category | ||||||
| Professional | ||||||
| Student demonstrates respect for other students and faculty members. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student upholds the dress code on campus and/or clinical sites. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student is prompt and on time for classes and all activities associated with clinical rotations. Demonstrates minimal class disruption and maximum commitment and respect to the lecturer by minimizing missed class sessions, late arrivals or early departures. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student refrains from unprofessional behaviors such as talking repetitively in class during lectures/labs/grand rounds etc. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student is able to work cooperatively, preserving relationships with peers and other members of the health care team. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates full understanding of HIPAA standards, including utilization of all media devices that place patients/providers at risk. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student refrains from personal cell phone usage during rotations or class, except to utilize program/facility approved medical apps for the sole purposes of accessing info for pt. care | 5 | 4 | 3 | 2 | 1 | N/A |
| Academic | ||||||
| Student demonstrates the ability to learn and function in a wide variety of didactic and clinical settings. This includes demonstration of ongoing learning by referencing didactic content and utilizing rotation unique study references, to keep pace with evolving standard of care practices. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates effective oral, electronic and written communication, addressing individuals utilizing appropriate tone and etiquette as well as grammar. (ex. using Dr. Miss, Mrs. Etc.) | 5 | 4 | 3 | 2 | 1 | N/A |
| Student exhibits academic integrity. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates adaptability. | 5 | 4 | 3 | 2 | 1 | N/A |
| Clinical | ||||||
| Student demonstrates patient safety practices and avoided putting patients’ well-being in jeopardy. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student upholds ethical standards of health care. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student provides competent medical care, under the supervision of an assigned preceptor and extends to each patient the full measure of their professional ability as dedicated, empathetic student healthcare providers. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student demonstrates the ability to adapt to, learn from and excel in a wide variety of dynamic settings. | 5 | 4 | 3 | 2 | 1 | N/A |
| Student is engaged in scholarly learning by coming to clinical rotations prepared to ask and answer questions and to actively participate in all learning opportunities. | 5 | 4 | 3 | 2 | 1 | N/A |
| Comments |
|
Faculty Advisor Signature: _______________________ Date: _________
Student Signature: ________________________ Date: _________
| PB1, ICS 2 | Demonstrate compassion, academic integrity, respect for others, intellectual honesty, and professional conduct. | ||||
| Expected behaviors include: | Level 1* | Level 2 | Level 3 | Level 4 | Level 5 |
| Respect for students, faculty, and staff Collaborative/cooperative Engaged No unnecessary conversation in class/labs/practicums, etc Academic integrity | Describes professional values and conduct with peers and supervisors. | Exemplifies professional values and conduct with peers and supervisors. | Exemplifies professional values and conduct with patients, peers, and supervisors. | Role model for professional values and conduct with patients, peers, and supervisors. | Coaches others in professional values and conduct. |
| PB1, CRPS 4 | Give and receive constructive feedback. | ||||
| Expected behaviors include: | Level 1* | Level 2 | Level 3 | Level 4 | Level 5 |
| Submit end-of-course evaluations When giving feedback, is specific, focused, and objective When receiving feedback, accepts responsibility and demonstrates respect | Accepts responsibility for personal and professional development by establishing goals. Identifies areas of strengths and opportunities in others | Respectfully gives feedback regarding strength and opportunities of others Demonstrates openness to performance data (feedback and other input) in order to inform goals | Intermittently seeks additional performance data with adaptability and humility Respectfully and appropriately offers guidance to others Offers guidance and feedback regarding institutional strengths and opportunities | Consistently seeks performance data with adaptability and humility Offers guidance and feedback regarding institutional strengths and opportunities | Leads performance review processes |
| PB 1, ICS 2 | Demonstrate basic PA professional responsibilities. | ||||
| Expected behaviors include: | Level 1* | Level 2 | Level 3 | Level 4 | Level 5 |
| Positive attitude Dress according to accepted standards Timely (on time for class/clinic and with assignments) Reliable (i.e. informing of status changes, concerns, fulfills obligations) Communicate effectively both verbally and written (tone, respectfully, timely, etc) | Takes responsibility for failure to complete tasks and responsibilities, identifies potential contributing factors, and describes strategies for ensuring timely task completion in the future Responds promptly to requests or reminders to complete tasks, responsibilities | Performs tasks and responsibilities in a timely manner with appropriate attention to detail in routine situations Recognizes situations that may impact won ability to complete tasks and responsibilities in a timely manner | Performs tasks and responsibilities in a timely manner with appropriate attention to detail in complex or stressful situations Proactively implements strategies to ensure that the need of patients, teams, and systems are met | Recognizes and addresses situations that may impact others’ abilities to complete tasks and responsibilities in a timely manner. | Leads teams to evaluate and change system outcomes and PA practice |
| PB 1, ICS 2 | Practice flexibility and maturity in adjusting to change. | ||||
| Expected behaviors include: | Level 1* | Level 2 | Level 3 | Level 4 | Level 5 |
| Emotional maturity, stability (resiliency, appropriate responses despite emotional triggers) Altruism Flexibility in learning in a variety of settings Self-aware, accountable to self Adaptability to changing information, environments, and situations | Identify potential triggers for personal lapses in flexibility and maturity in adjusting to change. Demonstrate maturity and flexibility in routine situations most of the time | Demonstrate flexibility and maturity in routine situations. | Demonstrate flexibility and maturity in complex or stressful situations. | Recognize situations that may trigger lapses and intervene to prevent lapses in one’s own flexibility and maturity in adjusting to change. | Mentor others in the practice of flexibility and maturity in adjusting to change. |
*Students scoring a level 1 of competency in any of the PDAT assessed subcompetencies will be considered for further review by the Student Progress Committee.
Students must score level 2 of competency at the time of promotion to the clinical year.
Students must score level 3 of competency in all areas to be eligible for program completion and graduation.
Student Name: Date:
Cumulative GPA:
| Program Requirement (73% or better in each course) | Date Completed |
| Semester 1 | |
| ☐ M500 ☐ M505 ☐ M509 ☐ M510 ☐ M531 ☐ D528 ☐ PDAT 2+ | |
| Semester 2 | |
| ☐ M501 ☐ M507 ☐ M818 ☐ M532 ☐ PDAT 2+ | |
| Semester 3 | |
| ☐ M502 ☐ M508 ☐ M696 ☐ PDAT 2+ | |
| Semester 4 | |
| ☐ M503 ☐ M504 ☐ M506 ☐ M694 ☐ PDAT 2+ | |
| Professionalism self-assessment | |
| PACKRAT I | |
| End of Didactic competency self-assessment | |
| Outstanding Requirements | |
| Successful Remediation | |
This student has met all program requirements to progress into the clinical year.
Program Director: SPC Chair:
Advisor: Student:
STUDENT NAME:
Rate your strength in each of the competencies using the following scale:
| 1 = Novice | 2 = Advanced Beginner | 3 = Competent | 4 = Proficient | 5 = Expert |
| OVERALL COMPETENCY MILESTONES | |||||
| CLINICAL AND TECHNICAL SKILLS | |||||
| CTS 1: Perform clinical and technical skills including procedures with appropriate supervision. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CTS 2: Perform complete and focused physical examinations. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
CLINICAL REASONING AND PROBLEM SOLVING | |||||
| CRPS 1: Order and interpret diagnostic studies. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 2: Generate a differential diagnosis and select the most likely diagnosis. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 3: Develop and carry out patient management plans. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 4: Identify and perform learning activities that address one’s gaps in knowledge, skills, and attitudes. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| INTERPERSONAL AND COMMUNICATION SKILLS | |||||
| ICS 1: Gather essential and accurate information about patients and their condition through medical history taking. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| ICS 2: Communicate effectively with other healthcare professionals. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| ICS 3: Maintain clear, accurate, timely, and legible medical records. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| MEDICAL KNOWLEDGE | |||||
| MK 1: Demonstrate the acquisition of broad-based medical knowledge in all major human organ systems. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| PROFESSIONAL BEHAVIORS | |||||
| PB 1: Display professional and ethical behaviors consistent with the PA profession. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
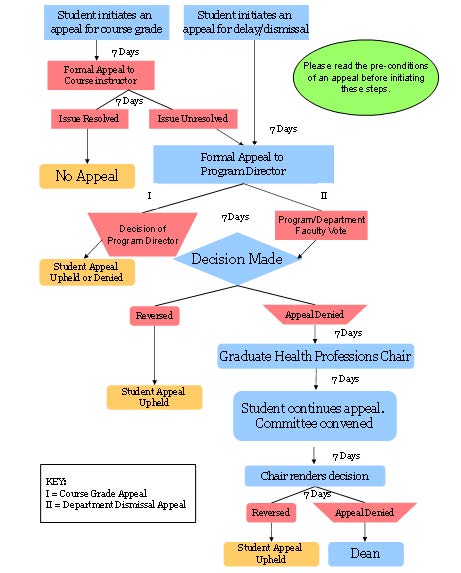
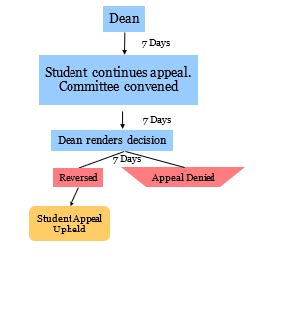
To initiate appeal for course grade:
- If a student would like to appeal a course grade, they must initiate a formal appeal to the course instructor.
- The course instructor has 7 days to resolve the issue.
- If issue is resolved, then there’s no need for the appeal to move forward.
- If the issue is unresolved once 7 days have passed, the formal appeal goes to the program director.
- Upon receipt of the student appeal, the program director has 7 days to review the appeal and make a decision or convene department faculty to determine merit of the appeal.
- The program director must respond to the student in writing on the outcome of the appeal at the department/program level within 7 days of receipt of the student appeal.
- In the event the program’s decision is to reverse the initial decision, then the student's appeal is upheld, and the corrective action is initiated.
- In the event the program does not overturn the decision and the appeal is denied, the student is entitled to take their appeal to the department level to request a review of the program decision.
- The chair then makes a decision on whether the student appeal is denied or upheld
- If appeal is denied, it goes to the Dean for review
To initiate appeal for delay/dismissal:
- Student initiates appeal if he/she wants to appeal a program dismissal or delay.
- Upon receipt of the student appeal, the program director has 7 days to review the appeal and make a decision or convene department faculty to determine merit of the appeal.
- The program director must respond to the student in writing on the outcome of the appeal at the department/program level within 7 days of receipt of the student appeal.
- In the event the program’s decision is to reverse the initial decision, then the student's appeal is upheld, and the corrective action is initiated.
- In the event the program does not overturn the decision and the appeal is denied, the student is entitled to take their appeal to the department level to request a review of the program decision.
- The chair then makes a decision on whether the student appeal is denied or upheld
- If appeal is denied, it goes to the Dean for review
Dean’s review:
Student initiates appeal at this level if they are dissatisfied with the appeal outcome at the Department/Program level (II)
- The student submits a letter requesting review of the program’s decision to the SHHS Dean within 7 days of the program decision.
- The appeals committee has 7 days to review the appeal and complete a written report. To facilitate review of the appeal, the appeals committee may interview the student or other involved parties and request any additional information that would assist the committee in their decision.
- The Dean receives the appeals committee’s recommendation and renders a decision within 7 days of receiving the recommendation and completes Section 3 of the Appeals routing form. The Dean then informs the student, the program, and the members of the appeals committee of the decision. The final copy of the original Appeals Routing form and all supporting documents are kept on file in the SHHS administrative office, with a copy provided to the program.
- The final decision in matters related to the program or academic policy rests with the School of Health & Human Sciences Office of the Dean.
Indiana University and IU Indianapolis each have a wide variety of academic resources available to students. This section highlights some of the resources most likely to be of value to you.
STANDARD A1.04The sponsoring institution must provide academic and student services to PA students that are equivalent to those services provided other comparable students of the institution.
Academic Tutoring
The IU Indianapolis University Writing Center is available to assist students with research papers:
University Writing Center
Phone: 317.274.2049
Website: https://liberalarts.indianapolis.iu.edu/programs/uwc/index.html
For assistance with medical documentation, students should consult with their Faculty Advisors.
SHHS Advising & Career Development
SHHS Advising & Career Development is available to assist students in preparing you for what comes next. School of Health & Human Sciences (SHHS) career experts are here to support your career development. If you’re exploring career options, developing career-ready skills, or engaging with potential employers, we are here for you.
SHHS Advising & Career Development
https://shhs.indianapolis.iu.edu/student-center/advising/index.html
Computer Labs
Computers for student use may be found on both the main campus and at medical libraries. Student Technology Centers (STCs) on campus are student computing facilities located mostly in classroom buildings on campus.
Computer locations and their availability may be found at:
https://uits.iu.edu/services/computer-labs/index.html
Disability Services
Students at IU Indianapolis who have a physical, medical, learning or psychiatric disability, either temporary or permanent, may be eligible for reasonable accommodations at the University as per the Americans with Disabilities Act (ADA) and/or Section 504 of the Rehabilitation Act. In order to receive such accommodations, students must identify themselves to the Adaptive Education Services (AES) Direct, and provide appropriate documentation and collaborate with the development of an appropriate accommodation plan.
Adaptive Education Services (AES) at IU Indianapolis provides a wide range of services for qualifying students, faculty, and staff with disabilities, as well as comprehensive accessibility evaluation and consulting services for the entire IU community.
Adaptive Education Services
Phone: 317.274.3241
Website: https://studentaffairs.indianapolis.iu.edu/care-support/accessible-educational-services/index.html
Financial Aid
The primary purpose of financial aid is to provide assistance to students who otherwise would be unable to pursue their education due to financial constraints.
The basic premise of financial aid programs is that the primary responsibility for meeting college costs lies with the student and student’s parents. When the family is unable to meet the cost of attendance, the Director of Student Financial Services will do its best to assist students in obtaining the necessary aid. The Director of Student Financial Services at IU Indianapolis is dedicated to assisting students and their families with any issues that may arise as they work through the financial aid process.
Director of Student Financial Services
420 University Blvd., CE 250
Indianapolis, IN 46202-5145
Phone: 317.274.4162
Fax: 317.274.3664
Email: iuindy.gradaid@iu.edu
Website: https://graduate.indianapolis.iu.edu/admissions/financial-support/index.html
University Libraries
IU Indianapolis has a library system that has a variety of resources that students will find valuable. Group study rooms may be used on a first-come, first-served basis.
The University Library
Central Indiana's premier academic research library designed to serve the needs of the electronic age.
In addition to holdings of more than 650,000 volumes, subscriptions to 4,000 plus periodicals and journals, and a full range of reference materials, the library hosts more than 250 public computer stations that provide access to campus electronic resources, the catalog systems of regional academic libraries and the Internet.
The library also houses 1,700 study spaces, group study rooms, computer and general classrooms, meeting rooms, and a 100-seat multimedia auditorium.
The University Library: https://library.indianapolis.iu.edu/
Ruth Lilly Medical Library
The Ruth Lilly Medical Library is located at 975 West Walnut Street in the Medical Research building. The Library collection focuses on authoritative literature in biomedical research and clinical practice. Established in 1908, the Ruth Lilly Medical Library contains more than 245,000 volumes, with current subscriptions to approximately 1900 journals.
Ruth Lilly Medical Library: https://library.mednet.iu.edu/
Campus & Other Libraries
Herron Art Library: https://library.indianapolis.iu.edu/herron
Ruth Lilly Special Collections and Archives: https://library.indianapolis.iu.edu/special
IU Indianapolis, Indiana & Other Libraries: https://iucat.iu.edu/catalog
It is the policy of each graduate program within the Indiana University School of Health and Human Sciences to comply with the Americans with Disabilities Act, Section 504 of the Rehabilitation Act of 1973, and state and local requirements regarding students and applicants with disabilities. Under these laws, no otherwise-qualified and competent individual with a disability shall be denied access to or participation in services, programs and activities solely on the basis of the disability.
In accordance with federal regulations established by the Americans with Disabilities Act, the following standards are described to assist each candidate in evaluating their prospect for academic and clinical success.
Working as a medical professional is often physically, mentally and emotionally demanding. All students receive a copy of the Technical Standards for Admission & Retention prior to matriculation. A copy of these standards may be found in this section for future reference.
The Indiana University Master of Physician Assistant Studies Program faculty has specified the following non-academic criteria ("Technical Standards") which all applicants’/physician assistant students are expected to meet in order to participate in the IU Master of Physician Assistant Studies Program and the practice of medicine.
It is important that each student reads each standard carefully.
a) Observation:
The applicant/physician assistant student must be able to participate actively in all demonstrations and laboratory exercises in the basic medical sciences and to assess and comprehend the condition of all patients assigned to him or her for examination, diagnosis and treatment. Such observation and information acquisition usually requires the functional use of visual, auditory and somatic sensation.
b) Communication:
The applicant/physician assistant student must be able to communicate effectively and sensitively with patients in order to elicit information, describe changes in mood, activity and posture, assess non-verbal communications and be able to effectively and efficiently transmit information to patients, fellow students, faculty, staff and all members of the health-care team. Communication skills include speaking, reading and writing, as well as the observation skills described above.
c) Motor:
The applicant/physician assistant student must have sufficient motor function to elicit information from patients by palpation, auscultation, percussion and other diagnostic maneuvers, be able to perform basic laboratory tests, possess all skills necessary to carry out diagnostic procedures and be able to execute motor movements reasonably required to provide general care and emergency treatment to patients.
d) Intellectual-Conceptual, Integrative and Quantitative Abilities:
The applicant/physician assistant student must be able to measure, calculate, reason, analyze and synthesize. Problem solving, the critical skill demanded of physician assistants, requires all of these intellectual abilities. In addition, the applicant/physician assistant student must be able to comprehend three-dimensional relationships and to understand the spatial relationships of structures. The applicant/physician assistant student must have the capacity to perform these problem-solving skills in a timely fashion.
e) Behavioral and Social Attributes:
The applicant/physician assistant student must possess the emotional health required for full utilization of his or her intellectual abilities, the exercise of good judgment, the prompt completion of all responsibilities attendant to the diagnosis and care of patients and the development of mature, sensitive and effective relationships with patients and others. Applicants/physician assistant students must also be able to tolerate taxing workloads, function effectively under stress, adapt to a changing environment, display flexibility and learn to function in the face of uncertainties inherent in the clinical problems of many patients. Compassion, integrity, concern for others, commitment and motivation are personal qualities which each applicant/physician assistant student should possess.
-Adapted from the Indiana University School of Medicine Technical Non-Academic Standards
| COMPETENCY MILESTONE RATIONAL | ||||
| SCORE | BLOOMS LEVEL | DREYFUS STAGE | EXPERIENCE EQUIVALENCE | EXAMPLE OF EXPECTED BEHAVIORS |
| 1 = Novice | REMEMBER, UNDERSTAND | Rule driven, analytic thinking, little ability to prioritize information | EARLY DIDACTIC STUDENT | WHEN GIVEN A PERTINENT PHYSICAL EXAM FINDING, REMEMBER ASSOCIATED DIAGNOSIS |
| 2 = Advanced Beginner | UNDERSTAND, APPLY | Able to sort through rules based on experience; analytic and non-analytic for some common problems | CLINICAL YEAR STUDENT | APPLY DIDACTIC MEDICAL KNOWLEDGE TO A CLINICAL SCENARIO |
| 3 = Competent | ANALYZE, EVALUATE | Embraces appropriate level of responsibility; dual processing of reasoning for most common problems; can see big picture; complex problems default to analytic reasoning; performance can be exhausting | NEW GRADUATE PA | GENERATE A TREATMENT PLAN THAT MEETS PATIENT’S NEEDS AND ACKNOWLEDGES AREAS OF UNCERTAINTY |
| 4 = Proficient | EVALUATE, CREATE | More fully developed non-analytic and dual process thinking; comfortable with evolving situations; able to extrapolate; situational discrimination; can live with ambiguity | EARLY CAREER PA | INDEPENDENTLY MANAGES COMPLEX PATIENT PRESENTATIONS |
| 5 = Expert | CREATE | Experience in subtle variations; distinguishes situations | EXPERIENCED PA | PROVIDES LEADERSHIP AND EXPERTISE FOR HEALTH PROVIDER COLLEAGUES |
| UNABLE TO ASSESS | DID NOT OBSERVE, HAS NOT YET RECEIVED INSTRUCTION | |||
| OVERALL COMPETENCY MILESTONES | |||||
| CLINICAL AND TECHNICAL SKILLS | |||||
| CTS 1: Perform clinical and technical skills including procedures with appropriate supervision. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CTS 2: Perform complete and focused physical examinations. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CLINICAL REASONING AND PROBLEM SOLVING | |||||
| CRPS 1: Order and interpret diagnostic studies. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 2: Generate a differential diagnosis and select the most likely diagnosis. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 3: Develop and carry out patient management plans. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| CRPS 4: Identify and perform learning activities that address one’s gaps in knowledge, skills, and attitudes. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| INTERPERSONAL AND COMMUNICATION SKILLS | |||||
| ICS 1: Gather essential and accurate information about patients and their condition through medical history taking. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| ICS 2: Communicate effectively with other healthcare professionals. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| ICS 3: Maintain clear, accurate, timely, and legible medical records. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| MEDICAL KNOWLEDGE | |||||
| MK 1: Demonstrate the acquisition of broad-based medical knowledge in all major human organ systems. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| PROFESSIONAL BEHAVIORS | |||||
| PB 1: Display professional and ethical behaviors consistent with the PA profession. | |||||
| 1 – NOVICE | 2 – BEGINNER | 3 – COMPETENT | 4 – PROFICIENT | 5 – EXPERT | UNABLE TO ASSESS |
| DETAILED COMPETENCY MILESTONES | |||||
| CLINICAL AND TECHNICAL SKILLS | |||||
| CTS 1: Perform clinical and technical skills including procedures with appropriate supervision. | |||||
| 1 - Identifies the breadth of procedures that PAs perform Recognizes PA role in referring patients for ap-propriate procedural care | 2 - Identifies patients for whom a procedure is indicated and who is equipped to perform it Counsels patients about expectations for common procedures performed by PAs and consultants | 3-Demonstrates confidence and motor skills while performing procedures, including addressing complications Performs independent risk and appropriateness assessment based on patient-centered priorities for procedures performed by consultants | 4 - Identifies and acquires the skills to independently perform procedures in the current practice environment Collaborates with procedural colleagues to match patients with appropriate procedures, including declining support for procedures that are not in the patient’s best interest | 5 - Identifies procedures needed in future practice and pursues supplemental training to independently perform | UNABLE TO ASSESS |
| CTS 2: Perform complete and focused physical examinations. | |||||
| 1– Performs basic elements of a physical exam and identify common abnormalities. | 2 – Conducts a complete or focused physical exam and identify common abnormalities | 3 – Conducts complete and focused physical exams, in an organized, efficient, and fluid sequence, interpreting abnormalities and maintaining patient comfort | 4 – Conducts complete and focused physical exams, using technology-enhanced physical diagnosis tools where appropriate, interpreting abnormalities and maintaining patient comfort | 5 – Coaches other medical providers and learners in the acquisition of these skills. | UNABLE TO ASSESS |
| CLINICAL REASONING AND PROBLEM SOLVING | |||||
| CRPS 1: Order and interpret diagnostic studies. | |||||
| 1- Interprets results of common diagnostic testing | 2- Interprets complex diagnostic information | 3- Synthesizes complex diagnostic information accurately to reach high probability diagnoses | 4- Anticipates and accounts for errors and biases when interpreting diagnostic tests | 5- Pursues knowledge of new and emerging diagnostic tests. Demonstrates mastery in the teaching of medical learners. | UNABLE TO ASSESS |
| CRPS 2: Generate a differential diagnosis and select the most likely diagnosis. | |||||
| 1- Incorporates key elements of a patient story into an accurate depiction of their presentation | 2- Develops an analytic, prioritized differential diagnosis for common presentations | 3- Develops a prioritized differential diagnosis for complex presentations | 4- Synthesizes information to reach high probability diagnoses with continuous re-appraisal to minimize clinical reasoning errors | 5 - Engages in deliberate practice and coaches others to minimize clinical reasoning errors | UNABLE TO ASSESS |
| CRPS 3: Develop and carry out patient management plans. | |||||
| 1- Associates first line treatments with common medical conditions. | 2- Develops acute and chronic patient management plans. | 3- Develops and implements evidence-based acute and chronic patient management plans that are patient-centered and culturally sensitive | 4- Creates efficient and effective patient-centered management plans that consider cost and healthcare system barriers. | 5 - Coaches others to provide best practice patient management plans that improve patient safety and reduce medical errors. | UNABLE TO ASSESS |
| CRPS 4: Identify and perform learning activities that address one’s gaps in knowledge, skills, and attitudes. | |||||
| 1- Identifies the factors which contribute to gap(s) between expectations and actual performance | 2- Self-reflects and analyzes factors which contribute to gap(s) between expectations and actual performance | 3- Self-reflects, analyzes, and institutes behavioral change(s) to narrow the gap(s) between expectations and actual performance | 4- Challenges assumptions and considers alternatives in narrowing the gap(s) between expectations and actual performance | 5- Coaches others on reflective practice | UNABLE TO ASSESS |
| INTERPERSONAL AND COMMUNICATION SKILLS | |||||
| ICS 1: Gather essential and accurate information about patients and their condition through medical history taking. | |||||
| 1– Gathers basic histories from patients, families, and electronic health records. | 2– Gathers complete histories from patients, families, and electronic health records relevant to clinical presentation | 3– Gathers complete and focused histories from patients, families, and electronic health records in an organized manner relevant to clinical presentation | 4– Gathers complete and focused histories from patients, families, and electronic health records in an organized manner, appropriate to the clinical situation and the individual, interpersonal, and structural factors that impact health | 5– Coaches other medical providers and learners in the acquisition of these skills. | UNABLE TO ASSESS |
| ICS 2: Communicate effectively with other healthcare professionals. | |||||
| 1- Respectfully requests/receives a consultation in a simulated environment. Uses language that values all members of the health care team. | 2- Clearly and concisely requests/responds to a consultation in a simulated environment. Communicates information effectively with all health care team members. | 3- Checks understanding of consultation recommendations, whether received or provided, to ensure clarity and accuracy. Communicates concerns and provides feedback to peers and learners. | 4- Coordinates recommendations from different members of the health care team to optimize patient care, resolving Communicates feedback and constructive criticism to supervising individuals. | 5- Role models flexible communication strategies that value input from all health care team members, resolving conflict when needed. Facilitates regular health care team-based feedback in complex situations. | UNABLE TO ASSESS
|
| ICS 3: Maintain clear, accurate, timely, and legible medical records. | |||||
| 1- Accurately and timely records information in the patient record. | 2- Demonstrates organized diagnostic and therapeutic reasoning through notes in the patient record. | 3- Uses patient record to communicate updated and concise information in an organized format. | 4- Demonstrates efficiency in documenting patient encounters and updating record. | 5- Optimizes and improves functionality of the electronic medical record within their system. | UNABLE TO ASSESS |
| MEDICAL KNOWLEDGE | |||||
| MK 1: Demonstrate the acquisition of broad-based medical knowledge in all major human organ systems. | |||||
| 1- Demonstrates basic knowledge of medical science and clinical medicine | 2– Recognizes typical clinical presentations; Describes basic pathophysiology of common diseases and patient presentations | 3- Explains the causes (behavioral, develop-mental, genetic, microbiologic, neoplastic, toxic, environmental, and traumatic) of diseases, injuries, and functional deficits affecting all major organ systems pertaining to a patient’s presentation | 4- Describes the altered structure/function resulting from disease, injuries, and deficits affecting all major organ systems; Interprets the clinical, histopathologic, laboratory, and/or radiographic manifestations commonly seen in practice | 5- Expands the knowledge base through dissemination of original research | UNABLE TO ASSESS |
| PROFESSIONAL BEHAVIORS | |||||
| PB 1: Display professional and ethical behaviors consistent with the PA profession. | |||||
| 1- Describes and accepts responsibility to adhere to professional behavior and ethical principles. | 2- Exemplifies professional values and ethical principles when applied to straightforward situations. | 3- Applies ethical principles and professional behaviors complex situations. | 4- Models behavior for ethical, professional practice. | 5- Leads and guides policy and system changes regarding ethical and professional practice in the PA profession and patient care environment. | UNABLE TO ASSESS |

